New Neurosurgical Classification Reveals Pivotal Role of Glioma Volume Reduction
International team develops system for a standardised assessment of operative success in treating certain brain tumours
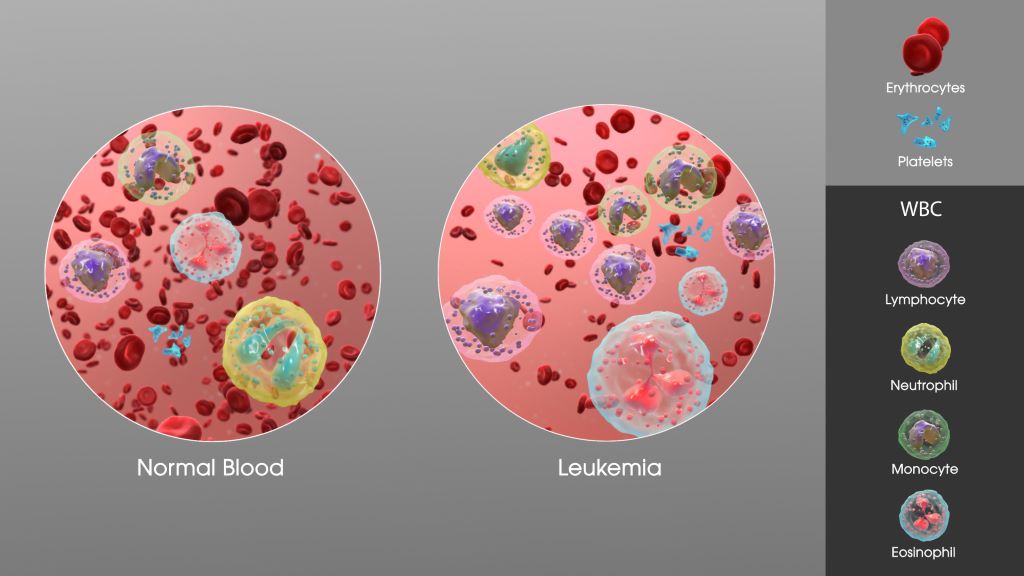
Low-grade brain tumours known as IDH-mutant gliomas CNS WHO grade 2 are life-threatening despite their slow growth. Neurosurgeons across the globe are faced with the question as to striking the correct balance between a “radical” tumour resection and avoiding further neurological damage. An international research team from the RANO working group involving Friedrich-Alexander-Universität Erlangen-Nürnberg (FAU) and Uniklinikum Erlangen has developed a new classification that records the extent to which any residual tumour tissue influences the progression of the disease. The results were published in The Lancet Oncology.
As a rule, the initial treatment for an IDH-mutated glioma CNS WHO grade 2 is surgery. The aim is to remove as much of the tumour as possible without jeopardising important neurological functions. As the results of the operation only become apparent many years later, there has been a lack of clear data, which has led to a number of different approaches. “On the one hand, this is due to the fact that we must be very careful to weigh up the chances of potentially boosting a patient’s chance of survival against avoiding neurological deficits. On the other hand, there has been a lack of clear criteria for assessing the risk of surgery until now, meaning that recommendations for treatment range from taking as little tissue as possible for diagnostic purposes to removing as much tumour tissue as possible,” explains Prof Dr Oliver Schnell from Uniklinikum Erlangen.
New basis for assessing success of surgery
In order to standardise therapeutic decisions, the RANO working group has conducted a large international study and assessed the data of 1391 patients from 16 neuro-oncological specialist units.
Based on the comprehensive data collected, the new RANO classification categorises the extent of the surgery based on the volume of the tumour that remains visible in a special MRI sequence (T2-FLAIR) after the operation. “Until now, there was no common language available for describing surgical outcomes,” explains PD Dr Philipp Karschnia from Uniklinikum Erlangen. “The new classification provides clarity, as it is guided exclusively by the residual tumour tissue.”
Less residual tumor means longer survival
The analysis of the RANO working group shows: A low volume of residual tumor after the initial operation is one of the most important factors for the further progression of the disease. A positive effect was also demonstrated for removing as much of the tumor as possible in the case of oligodendrogliomas, that tend to have a more favourable progression and are highly sensitive to chemo and radiation therapy. “We were surprised to discover that even follow-up treatments such as chemotherapy or radiation therapy were not able to replace the influence of the operation,” admits PD Dr Karschnia.
Internationally verified and useful in a wide range of scenarios
The results were confirmed in an independent patient group at the University of California in San Francisco. The new classification supports surgeons in making more accurate decisions and paves the way for future studies: “The new RANO classification is a milestone that will make a significant impact on neuro-oncological research and care in the long term,” according to Prof Schnell.
The Response Assessment in Neuro-Oncology (RANO) Working Group is an international, multidisciplinary collaboration between experts from various disciplines who have been working together to develop standardised criteria for assessing brain tumours for more than a decade now. Experts involved in the study from Erlangen were Prof Dr Oliver Schnell and PD Dr Philipp Karschnia, who has been leading the surgical focus group of the RANO Working Group since 2024, Dr Nico Teske and Alfred Gramelt from the Department of Neurosurgery at Uniklinikum Erlangen.