Drugging the Undruggable: A Million-fold Leap in Targeting Elusive Cancer Proteins
Few medications can target disordered proteins, but new research outlines an enhanced approach that could lead to treatments for prostate cancer and other diseases

Researchers at the University of British Columbia and BC Cancer have developed a new way to target proteins long considered ‘undruggable’, opening the door to new treatments for prostate cancer and other serious diseases.
Known as intrinsically disordered proteins, these molecular shapeshifters are extremely difficult to target with medication due to their flexible and ever-changing structure. They play a central role in a wide range of diseases, including cancer, neurodegenerative disorders, heart disease and autoimmune conditions, yet only a handful of medications currently exist that can target them.
In a study published today in Nature Signal Transduction and Targeted Therapy, the researchers demonstrate a new approach for designing drugs that bind more strongly to these proteins and block their disease-causing activity. In some cases, the compounds they developed bound up to a million times more tightly than any previously reported.
“This study shows that proteins previously thought to be undruggable can be drugged with remarkable efficacy,” said principal investigator Dr Marianne D. Sadar, professor of pathology and laboratory medicine at the UBC faculty of medicine and distinguished scientist at BC Cancer. “The findings could have profound implications for the treatment of cancer and other diseases, providing a roadmap for the development of new treatments.”
A long-standing challenge in drug discovery
Unlike most proteins, which fold into stable three-dimensional shapes, disordered proteins contain flexible regions that change as they interact with molecules inside cells. Because they lack fixed binding sites, they are extremely difficult to target with traditional drugs.
“Most drug discovery is like designing a key for a very specific lock,” said Dr Sadar. “But disordered proteins don’t behave like locks at all, they’re more like moving strands of spaghetti.”
Dr Sadar and her team have spent decades studying how to target these proteins. In 2008, they developed the first compound capable of binding to them, and have since advanced two such drugs into clinical trials – another world-first milestone for the field.
Despite these advances, achieving strong and consistent binding has remained a central challenge.
A new strategy against prostate cancer
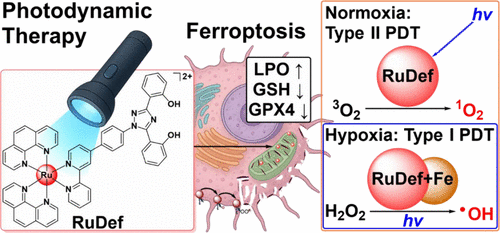
The new study focused on a specific protein, the androgen receptor, which fuels the growth of most prostate cancers.
Rather than fitting into a single fixed spot, the researchers developed compounds that interact with the moving region of the protein, freeze it in an inactive state, and prevent it from turning on genes that drive cancer growth.
“It’s a major achievement. Our target drugs had binding affinity a million times greater than existing drugs targeting these regions,” said Dr Natalie Strynadka, professor of biochemistry and molecular biology at the UBC faculty of medicine.
By systematically modifying the compounds at the molecular level, the researchers identified several promising candidates that effectively shut down the receptor. In animal studies, several compounds slowed prostate cancer growth more effectively than a commonly used prostate cancer treatment.
“What surprised us was how effectively these molecules could attach to a protein that doesn’t have a fixed structure,” said Dr Raymond Andersen, professor in UBC’s department of chemistry. “We were able to shut down the androgen receptor even in situations where current prostate cancer drugs stop working.”
The researchers now aim to advance the most promising candidates toward clinical trials, with the goal of developing prostate cancer drugs that can be used earlier in treatment and with fewer side-effects. Because disordered proteins are involved in many diseases, they say the approach could have a much broader impact.
“If the approach continues to prove successful, it could dramatically expand the number of proteins that scientists can target with medicines – turning what was once considered a dead end into a promising new frontier for drug discovery,” said Dr Sadar.
Source: University of British Columbia