New Treatment for Toxoplasmosis Could Target Parasite Cysts
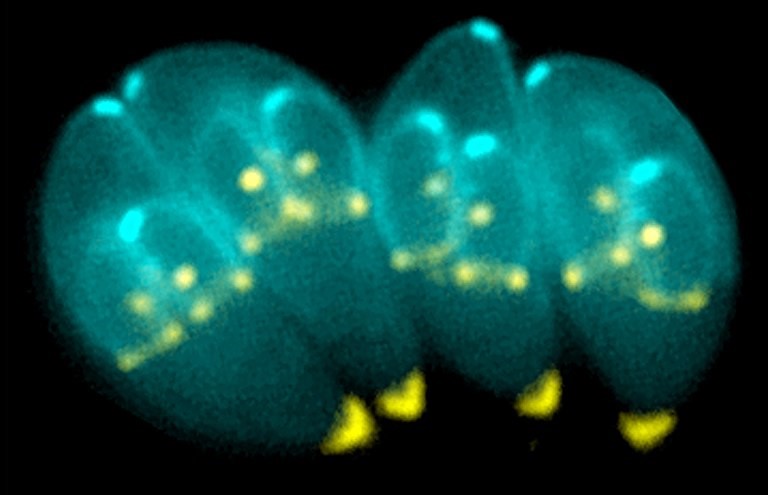
Findings from a new University of Kentucky College of Medicine study published in the Journal of Biological Chemistry could lead to a new treatment for Toxoplasma gondii, the parasite that causes toxoplasmosis.
An estimated 40 million people in the US carry the parasite T. gondii, according to the Centers for Disease Control and Prevention, but most are asymptomatic because the immune system usually keeps the parasite from causing illness. However, for women newly infected during pregnancy and anyone with a compromised immune system, toxoplasmosis can cause severe illness or even death.
In individuals with severe toxoplasmosis, cyst version of the parasite may be present within brain and muscle tissue. These cysts are responsible for causing serious disease, especially in people who are immunocompromised. While there are FDA-approved drugs to treat the symptoms of toxoplasmosis, no current therapeutics target the cyst form of the parasite.
The labs of Matthew Gentry, PhD, and Craig Vander Kooi, PhD, at UKCM and Zhong-Yin Zhang, PhD, at the Purdue Institute for Drug Discovery, collaborated to develop a drug that targets the cyst form of the parasite.
In previous research, Dr Gentry identified an enzyme in T. gondii called TgLaforin, which he hypothesised was critical in allowing the parasite to access energy from a carbohydrate storage molecule. The team developed a new drug that inhibits TgLaforin with the goal of preventing enzymes from accessing and providing energy to the parasite.
The new discovery was made possible thanks to the multidisciplinary collaboration of experts from the four labs, said Dr Gentry.
Robert Murphy, PhD, a member of the Gentry and Sinai labs, conducted initial experiments that characterised TgLaforin and provided a baseline for understanding the enzyme’s function.
Tiantian Chen, a graduate student in Vander Kooi’s lab, generated models of TgLaforin using a new program called AlphaFold2, an AI algorithm that provides valuable insights into research. Chen generated models that provided a picture of the enzyme that demonstrated TgLaforin was a unique and possible drug target.
Jianping Lin, PhD, a postdoc in Dr Zhang’s lab, then used information generated by Dr Murphy and Chen in combination with novel techniques in chemistry to generate the first version of a future anti-Toxoplasma drug.
“I was excited to find that the drug was effective against TgLaforin in test tubes and that it prevented TgLaforin from performing its normal activity against a variety of substrates, including carbohydrates,” said Dr Murphy.
The labs will next test the drug on parasites, and try to increase its potency and selectivity and adapt its chemical properties to allow for animal studies.
“This study is a great example of what Provost DiPaola consistently promotes regarding transdisciplinary research,” Dr Gentry said. “This work was a true team effort and it is very exciting to see where we take it next.”