Yawns in Healthy Foetuses Might Indicate Mild Distress
Foetuses yawn in the womb, with more yawns associated with a lower weight at birth

Even in the womb, where all oxygen is provided by the parental placenta, foetuses can – and do – yawn. More yawns during observation were associated with a lower weight at birth – potentially indicating mild foetal stress in the womb, according to a study published February 25, 2026 in the open-access journal PLOS One by Damiano Menin, of the Università degli Studi di Ferrara in Italy, and colleagues.
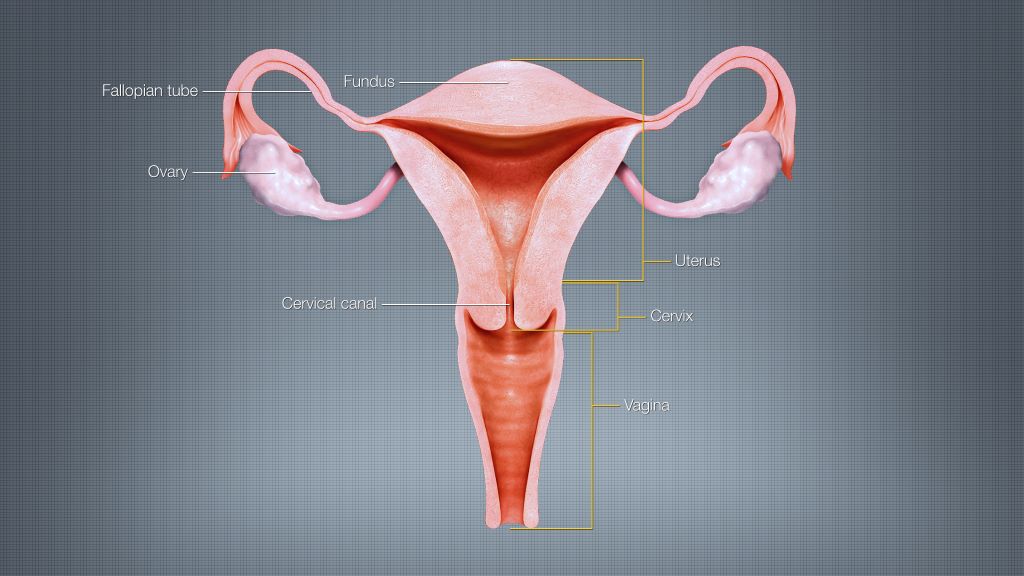
Yawning is a behaviour found across vertebrates – and no one quite knows why. In humans, foetuses yawn in the womb from about 11 weeks. Even though there is no air to breathe, they slowly open their mouths, make motions similar to inhalation and exhalation, and close their mouths again. To understand more about foetal yawns, the authors of this study used ultrasound to observe 32 healthy foetuses (56% female, 44% male) between 23 and 31 weeks. Each foetus was observed for 22.5 minutes.
The authors found that the foetuses yawned between zero and six times during the observation period, with an average of 3.63 yawns per hour. They also showed that foetuses that yawned more during their observations were more likely to have a low weight at birth, which is considered as an indicator of mild distress – though all foetuses in the study were born healthy.
The researchers did not perform any manipulations to see if they could affect foetal yawning and also did not record measures such as foetal heart rate or maternal temperature which might potentially be associated with the behaviour. Additionally, no high-risk pregnancies were observed. Based on their research, the authors suggest that frequent foetal yawning might be a sign of mild distress in the healthy foetus.
The authors add: “We found that yawning frequencies in the womb are negatively related to birth weight, potentially indicating a stress-related response in healthy fetuses. This suggests that even before birth, yawning may serve as an indicator of a foetus’s well-being.”
Provided by PLOS