Innovative Surgery Cuts Ovarian Cancer Risk by Nearly 80%
New research shows that Canadian-developed surgical procedure dramatically reduces rates of the most lethal gynaecological cancer
A prevention strategy developed by Canadian researchers reduces the risk of the most common and deadly form of ovarian cancer by nearly 80%, according to a new study published today in JAMA Network Open.
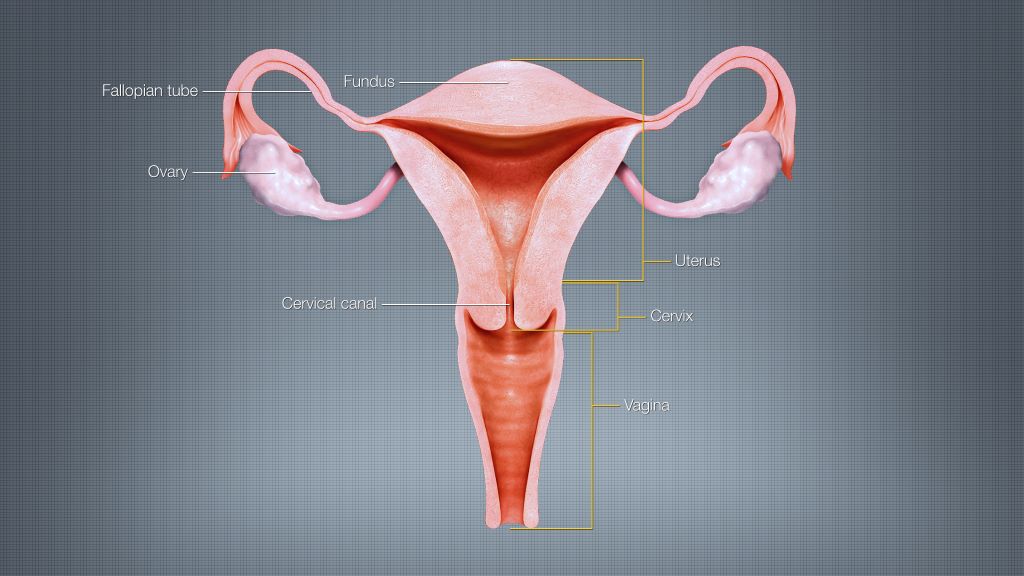
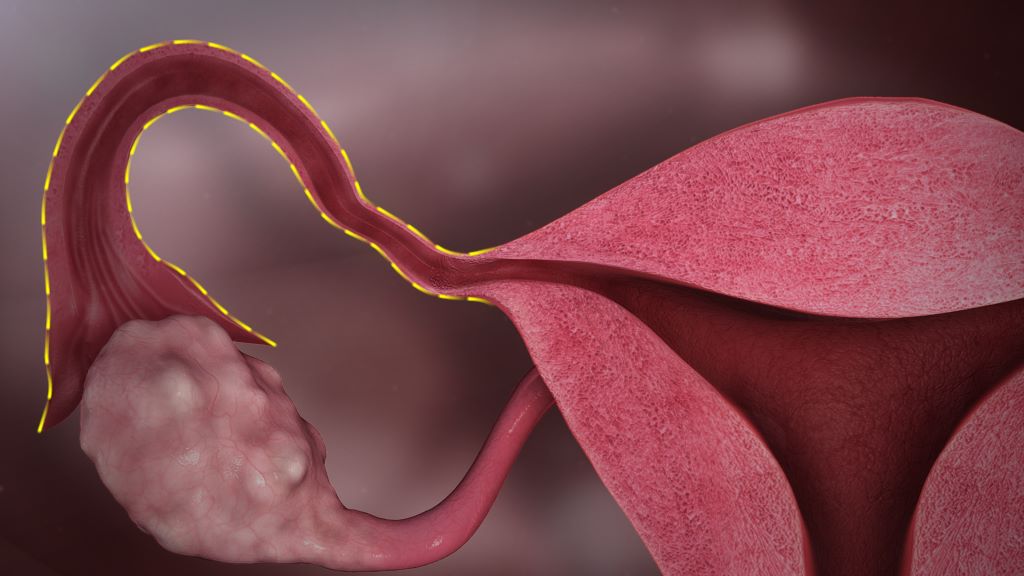
The strategy, known as opportunistic salpingectomy (OS), involves proactively removing a person’s fallopian tubes when they are already undergoing a routine gynaecological surgery such as hysterectomy or tubal ligation, commonly called “having one’s tubes tied”.
British Columbia in Canada became the first jurisdiction in the world to offer OS in 2010, after a team of researchers from UBC, BC Cancer and Vancouver Coastal Health designed the approach when it was discovered that most ovarian cancers originate in the fallopian tubes rather than the ovaries. OS leaves a person’s ovaries intact, preserving important hormone production so there are minimal side effects from the added procedure.
The new study, led by a B.C.-based international collaboration called the Ovarian Cancer Observatory, provides the clearest evidence yet that the Canadian innovation saves lives.
“This study clearly demonstrates that removing the fallopian tubes as an add-on during routine surgery can help prevent the most lethal type of ovarian cancer,” said co-senior author Dr Gillian Hanley, an associate professor of obstetrics and gynaecology at UBC. “It shows how this relatively simple change in surgical practice can have a profound and life-saving impact.”
New hope against a deadly cancer
Ovarian cancer is the most lethal gynaecological cancer. Approximately 3100 Canadians are diagnosed with the disease each year and about 2000 will die from it.
There is currently no reliable screening test for ovarian cancer, meaning that most cases are diagnosed at advanced stages when treatment options are limited and survival rates are low.
The OS approach was initially developed and named by Dr Dianne Miller, an associate professor emerita at UBC and gynaecologic oncologist with Vancouver Coastal Health and BC Cancer. She co-founded B.C.’s multidisciplinary ovarian cancer research team, OVCARE.
“If there is one thing better than curing cancer it’s never getting the cancer in the first place,” said Dr. Miller.
The new study is the first to quantify how much OS reduces the risk of serous ovarian cancer – the most common and deadly subtype of the disease. It builds on previous research demonstrating that OS is safe, does not reduce the age of menopause onset, and is cost-effective for health systems.
The study analysed population-based health data for more than 85 000 people who underwent gynaecological surgeries in B.C. between 2008 and 2020. The researchers compared rates of serous ovarian cancer between those who had OS and those who had similar surgeries but did not undergo the procedure.
Overall, people who had OS were 78% less likely to develop serous ovarian cancer. In the rare cases where ovarian cancer occurred after OS, those cancers were found to be less biologically aggressive. The findings were validated by data collected from pathology laboratories from around the world, which suggested a similar effect.
From B.C. innovation to global impact
Since its introduction in B.C. in 2010, OS has been widely adopted, with approximately 80 per cent of hysterectomies and tubal ligation procedures in the province now including fallopian tube removal.
Globally, professional medical organizations in 24 countries now recommended OS as an ovarian cancer prevention strategy, including the Society of Obstetrics and Gynaecology of Canada, which issued guidance in 2015.
“This is the culmination of more than a decade of work that started here in B.C.,” said co- senior author Dr. David Huntsman, professor of pathology and laboratory medicine and obstetrics and gynaecology at UBC and a distinguished scientist at BC Cancer. “The impact of OS that we report is even greater than we expected.”
The researchers say expanding global adoption of OS could prevent thousands of ovarian cancer cases worldwide each year.
“This is a powerful example of how UBC research is changing clinical practice worldwide and saving lives,” said Dr Sharmila Anandasabapathy, dean of the faculty of medicine and vice-president, health, at UBC. “It speaks to the strength of our researchers and clinicians working together to translate discovery into real-world impact for patients here at home and around the world.”
Extending OS to other abdominal and pelvic surgeries where appropriate could further increase the number of people who could benefit from the prevention strategy. B.C. recently became the first province to expand OS to routine surgeries performed by general and urologic surgeons through a project supported by the Government of B.C. and Doctors of BC.
“Our hope is that more clinicians will adopt this proven approach, which has the potential to save countless lives,” said Dr Huntsman. “Not offering this surgical add-on may leave patients unnecessarily vulnerable to this cancer.”
Brett Goldhawk
Source: University of British Columbia