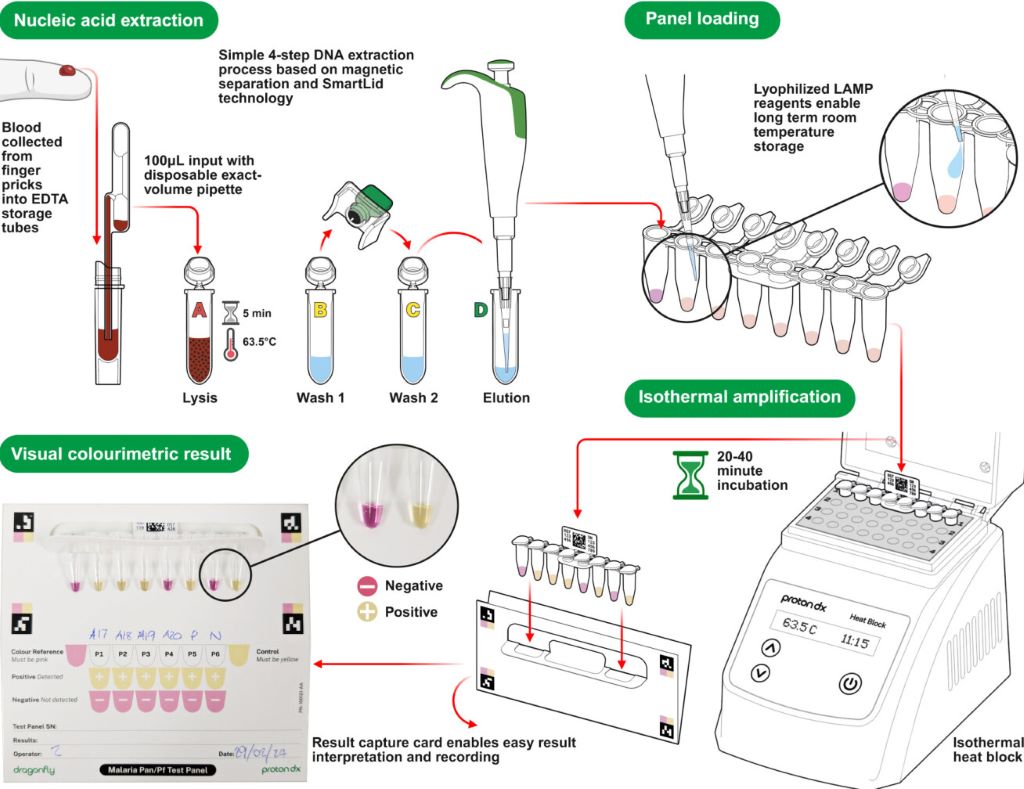
Ivermectin Was Touted as a Cure for COVID, Now it’s Being Tested for Cancer. But what can it Actually Treat?
Nial Wheate, Macquarie University
Ivermectin was originally celebrated as a revolutionary treatment for parasitic disease in humans and animals. It has since evolved into a focal point of misinformation and heated debate.
During the early part of the COVID pandemic, it was touted on social media as a miracle cure for the virus, despite a lack of robust evidence.
Now the United States National Cancer Institute is looking into the drug as a potential cancer treatment, with early human clinical studies underway.
But what can it successfully treat?
What is ivermectin?
The drug is a small organic chemical that can be extracted from the bacterium Streptomyces avermitilis. This bacterium grows in the soil, and was first found near the grounds of a Japanese golf course.
Ivermectin’s discovery in the 1970s was considered so important its discoverers were awarded the 2015 Nobel Prize in Physiology or Medicine.
It was first approved for use in animals in 1981 and in humans in 1987. It’s now available in various brands as tablets and creams you apply to the skin.
Assessing the evidence
Governments use human clinical trials to decide whether to approve a medicine for sale.
But clinical trials aren’t the highest level of evidence to inform best practice and guide decisions. For that, there are Cochrane reviews.
A Cochrane review brings together a panel of experts who collate and assess all the relevant evidence on a medication. It takes data from multiple clinical trials, and other studies, and evaluates it following clear and structured steps. It’s able to examine and critique study designs to identify bias and reject bad data.
Cochrane reviews are also regularly updated to take into account new information. The result is a summary that is considered the highest level of evidence to guide decision-making.
So what do Cochrane reviews say about ivermectin for different conditions?
What can and can’t ivermectin treat?
| Condition | Does it work? | Notes |
|---|---|---|
| Cancer | Unclear | Studies only just starting |
| COVID | No | Does not prevent infection or treat |
| Gut and lymphatic worms | Yes | Treatment for various roundworms |
| Malaria | Unclear | Not enough evidence to decide |
| River blindness | Unclear | Not enough evidence to decide |
| Rosacea | Yes | Use the topical formulation |
| Scabies | Yes, but with caveats | Not the most effective |
Gut and lymphatic worms
Ivermectin is used to treat a variety of parasitic worm infections. These include the round worms Ascaris lumbricoides, Strongyloides stercoralis, Wuchereria bancrofti, and Brugia malayi.
The latter two worms cause the disease lymphatic filariasis (or elephantiasis) which causes severe swelling in the arms, legs, breasts and genitals.
When ivermectin is used to treat Strongyloides stercoralis, the Cochrane panel found it is better than albendazole and had fewer side effects than thiabendazole.
For Ascaris lumbricoides, the panel concluded ivermectin was as good as albendazole and mebendazole.
For treating lymphatic filariasis, a Cochrane review found ivermectin or diethylcarbamazine should be standard treatment in combination with albendazole.
Rosacea
The Cochrane review for rosacea evaluated 22 different treatments for this skin condition, including a variety of drugs, as well as light therapy, cosmetics and reducing the intake of spicy food.
It concluded that ivermectin applied to the skin was more effective than a placebo, and a bit better than the other standard medication, metronidazole.
Scabies
Cochrane has two reviews on the use of ivermectin for scabies. One specifically evaluated ivermectin and permethrin as treatments. The other evaluated all available treatments for scabies.
The first review concluded both permethrin and ivermectin were just as effective, regardless of whether the ivermectin was administered orally or directly onto the skin.
In contrast, the second review concluded ivermectin does work but topical permethrin appeared to be the most effective treatment.
Malaria
The Cochrane panel looked specifically at whether ivermectin could reduce transmission of the malaria parasite, rather than as a treatment.
Unfortunately there was just a single clinical trial to use as evidence. In that trial, residents of eight villages were given ivermectin and albendazole together, with follow up doses of just ivermectin. The researchers then looked at the rates of child infection over 18 weeks.
Even though the trial didn’t show ivermectin prevented infection, due to the high risk of bias in it, the Cochrane panel couldn’t conclude either way whether ivermectin worked or not.
River blindness
River blindness is caused by another parasitic worm called Onchocerca volvulus.
The Cochrane review concluded there was a lack of evidence either way to know whether it works to prevent infection-based visual impairment and blindness.
It evaluated the data from four clinical trials and two large community-based studies.
One of the reasons the panel was unable to make a firm conclusion was because it thought the drug may work differently against different strains of the parasite and in people of different ethnicity.
Cancer
There are no Cochrane reviews on ivermectin’s use for cancer because clinical interest in the drug for this condition is just starting.
There is a current clinical trial that is evaluating ivermectin in combination with antibody-based drugs for breast cancer.
Early results showed the combination of antibody drugs with ivermectin was safe to patients, but no efficacy data has been published.
COVID
The Cochrane panel rejected the data for seven clinical trials and included 11 other trials. Rejected trials included those which compared ivermectin against other drugs which were known to not be effective against COVID, such as hydroxychloroquine.
The review concluded there was no evidence to support the use of ivermectin for the treatment or prevention of COVID. In making that conclusion, it evaluated treatments that used invermectin or placebo in combination with standard care and whether treatment reduced death, illness, or the length of the infection.
Nial Wheate, Professor, School of Natural Sciences, Macquarie University
This article is republished from The Conversation under a Creative Commons license. Read the original article.