Researchers Pioneer New Breathing Test to Detect Lung Disease Earlier
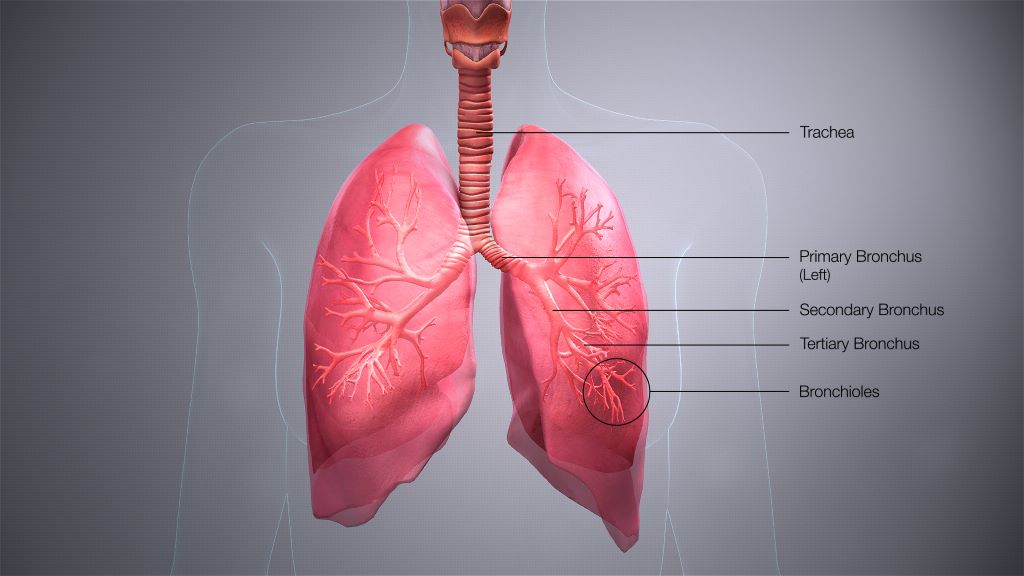
A new project led by Oxford University aims to develop a novel breathing test that could detect asthma and COPD earlier, more accurately, and closer to home – reducing pressure on the NHS and improving outcomes for patients.
This work is included in a portfolio of research funded by the Engineering and Physical Sciences Research Council (EPSRC), part of UK Research and Innovation, to make diagnostic testing more accessible by designing simple, affordable tools that can be used in everyday settings. The project, called ACCESS (A Community-based diagnostiC for early airwayS disease), focuses on airway diseases, and will receive £1.3 million over three years.
Chronic respiratory diseases such as asthma and chronic obstructive pulmonary disease (COPD) affect more than half a billion people worldwide and cause over four million deaths every year. In the UK, these conditions hit disadvantaged communities hardest, with people in areas of socioeconomic deprivation facing particular challenges in accessing hospital-based diagnostic care.

Currently, asthma and COPD diagnosis relies on a test called spirometry. This measures how much air a person can forcefully breathe out, but it is difficult for many patients to perform and often fails to detect disease in its earliest stages. By the time spirometry picks up abnormalities, damage to the lungs is usually irreversible, resulting in late diagnoses, missed chances for early treatment, and poorer outcomes.
The project is enabled by the strong ethos for collaborative and innovative research in this University and will be delivered by a multi-disciplinary team, working across university departments and the NHS.
Project lead Professor Grant Ritchie
To address these issues, Oxford researchers have developed a new test, known as computed cardiopulmonography (CCP), that could transform the way lung diseases are diagnosed. CCP is performed while a patient breathes normally for 12 minutes through a mouthpiece linked to a highly accurate gas analyser. Using cutting-edge laser technology and advanced mathematical modelling, the test captures a detailed picture of how evenly air flows through the lungs. This “fingerprint” of lung function changes early in the course of disease, making CCP a powerful tool for spotting subtle problems that spirometry can miss.
Early studies in people with asthma, COPD, and even in otherwise healthy smokers suggest CCP is a highly sensitive marker of small airways damage. But while the results are promising, the test currently takes too long and requires specialist gas supplies, restricting its use to hospitals and research labs.
The goal of the ACCESS project is to adapt CCP for community use, for instance in GP surgeries, pharmacies, and community diagnostic hubs. Specifically, the research team will work to reduce the time duration and volume of gas needed for each test, and speed up the data analysis so that results can be shared with the patient during the same appointment. Towards the end of the project, CCP will be trialled in a community diagnostic centre to gather feedback from patients and healthcare professionals.
The long-term goal is to support earlier diagnosis and treatment, helping reduce hospital visits and tackle health inequalities. By enabling earlier intervention and delivering care closer to home, CCP has the potential to improve outcomes for millions of people living with lung disease.
Source: Oxford University







 PRO check prototype one demonstrated how laser gridlines and a camera can be used to image the surface of the prostate.
PRO check prototype one demonstrated how laser gridlines and a camera can be used to image the surface of the prostate.
