A Simple Neck Scan Could Detect Men at High Risk of Heart Failure
A simple neck scan can identify men with double the risk of heart failure, according to a new study led by UCL researchers and funded by the British Heart Foundation and the National Institute for Health and Care Research.
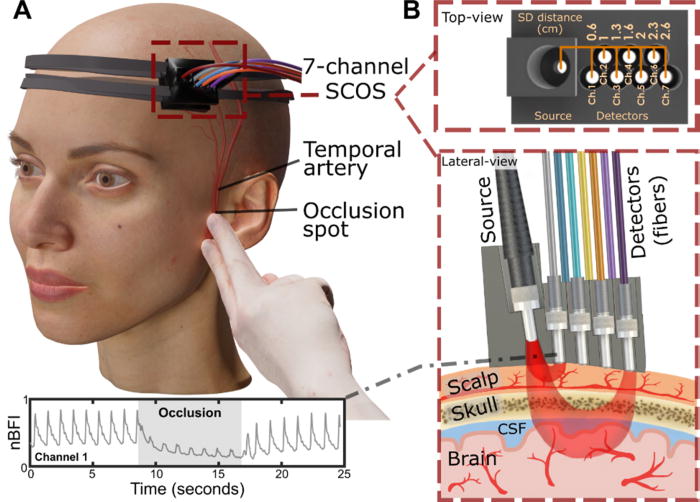
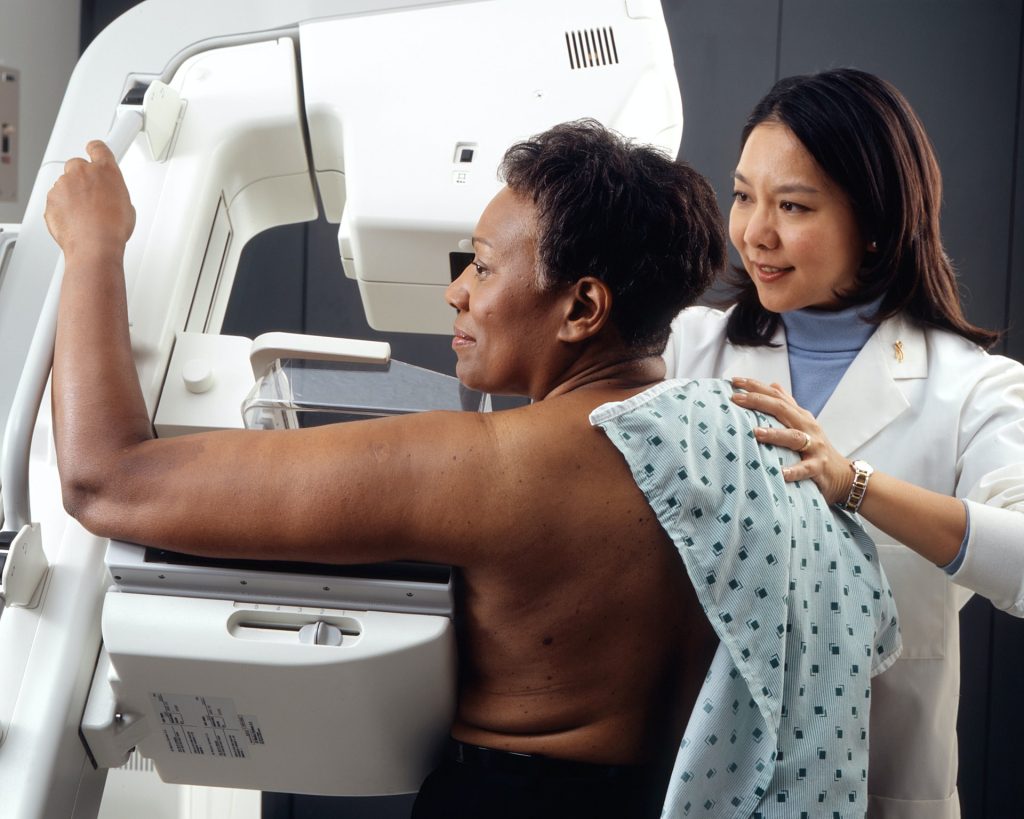
A carotid ultrasound, like the ultrasound for pregnant women, is quick and painless, using a small handheld device moved gently over the neck to scan the arteries underneath.
When around 1600 men over the age of 70 received the scan, it showed the ‘flexibility’ of their carotid arteries – how much they stretch and expand with each heartbeat.
Researchers found that the quarter of men with the least flexible carotid arteries were 2.5 times more likely to develop heart failure than those with the most flexible carotid arteries.
These people could be encouraged by doctors to eat more healthily, do more exercise and take medications, if needed, to help reduce their risk of developing heart failure.
GPs do not currently routinely carry out the cheap and easy scan on healthy patients without symptoms. But, where GP surgeries have the capacity, offering a neck scan to older people to measure the flexibility of their arteries could help them better understand their risk of future heart failure, according to the researchers.
Having relied upon data from the British Regional Heart Study, which began in the 1970s and only involved men, researchers highlight that these findings next need to be looked at in women.
Dr Atinuke Akinmolayan (UCL Primary Care & Population Health), who is now a GP, said: “The carotid ultrasound is a safe, cheap and painless investigation, and our findings suggest it may be able to provide an early warning sign for heart failure.
“More research is needed, especially to see if this works for women, but this is something GPs could look at offering to people over the age of 60, where possible and believed needed.
“A patient who gets an ultrasound result indicating they may be at higher risk of future heart failure could have an important conversation with their doctor about lifestyle changes they could make to lower that risk.”
Doctors tend to scan the two carotid arteries, which run up either side of the neck, when someone has had a stroke or is at risk of a stroke following a transient ischaemic attack, known as a ‘mini-stroke’. A scan can identify carotid artery disease – a build-up of fatty material which can cause a stroke by breaking off and travelling into the brain or by narrowing the arteries and stopping blood reaching the brain.
However, the carotid arteries may be a red flag for heart failure also. This is because, when the carotid arteries become less flexible, they do not expand properly to let blood through. This can raise blood pressure, which forces the heart muscle to work harder. Over time, this can lead to heart failure.
The study, published in the Journal of the American Heart Association, looked at 1631 British men, aged 71 to 92, who had a carotid artery ultrasound between 2010 and 2012 as part of the British Regional Heart Study.
A carotid ultrasound, sometimes called a Doppler scan, takes an average of 15 to 30 minutes for most people, although this can vary.
A small handheld sensor is moved back and forth over the neck, generating sound waves which bounce off the arteries. That provides an echo which changes in frequency when blood flow is reduced in the blood vessels because they are narrowed by built-up fatty material.
The narrowing identified by a carotid scan can then be used to calculate the arteries’ flexibility, after factoring in other measures, including blood pressure. Researchers were able to identify the quarter of men with the least flexible carotid arteries, and the quarter of men whose carotid arteries were most flexible.
They then compared the rates of heart failure in each group over an average of six years after their neck scans.
Even after considering other causes of heart failure, like age, weight, smoking and whether people had previously suffered a heart attack, the quarter of men with the least flexible carotid arteries had 2.5 times the risk of developing heart failure, compared to the quarter with the most flexible carotid arteries.
In a separate finding, looking at the thickness of people’s carotid arteries rather than their flexibility, the study found that men with thicker carotid arteries were more likely to have a heart attack or die from one.
For every ‘unit’ increase in the thickness of the carotid artery wall – with a unit equalling 0.16 millimetres – the risk of having a heart attack increased by about 29 per cent, even after considering other relevant factors like age and weight.
However the thickness of the carotid arteries was not found to be significantly linked to future heart failure in the study.
There are around 200 000 new cases of heart failure diagnosed every year in the UK.
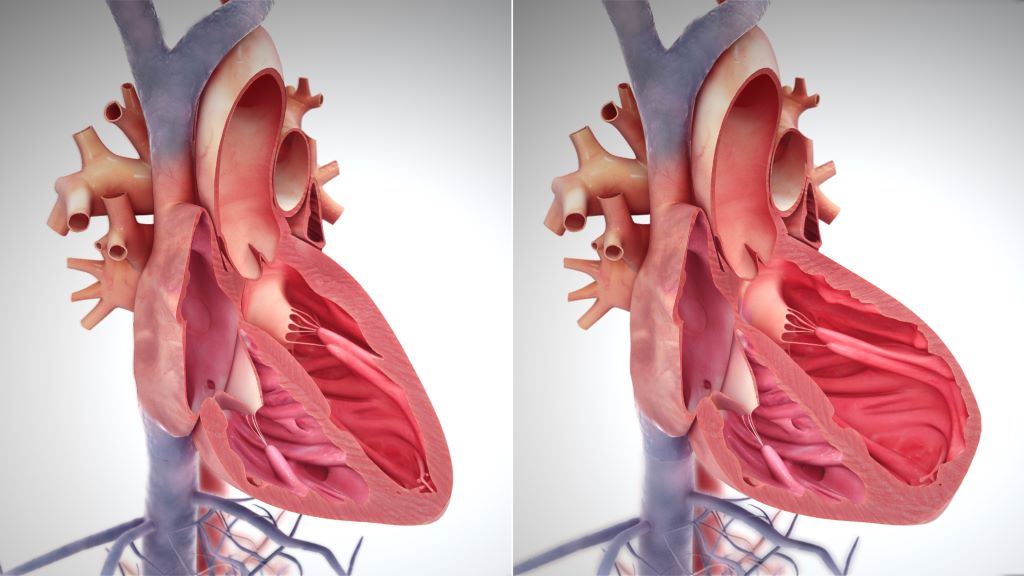
It occurs when the heart is not pumping blood around the body as well as it should, most commonly when the heart muscle has been damaged – for example, after a heart attack.
Heart failure can cause extreme fatigue, shortness of breath and fainting.
Professor Bryan Williams, chief scientific and medical officer at the British Heart Foundation (BHF), who is also Chair of Medicine at UCL Institute of Cardiovascular Science, said: “The findings of this study are interesting and show that stiffening of arteries is associated with increased risk of heart failure, most likely due to the heart having to work harder against the resistance caused by these stiffer arteries.
“It is an important signal that whenever we detect such changes in the carotid arteries, we should also be thinking of the potential impact on the heart and an increased risk of heart failure – which we have treatment strategies to prevent.”
Source: University College London