Study Reveals Unseen Changes in Motor Control After Spinal Cord Injury
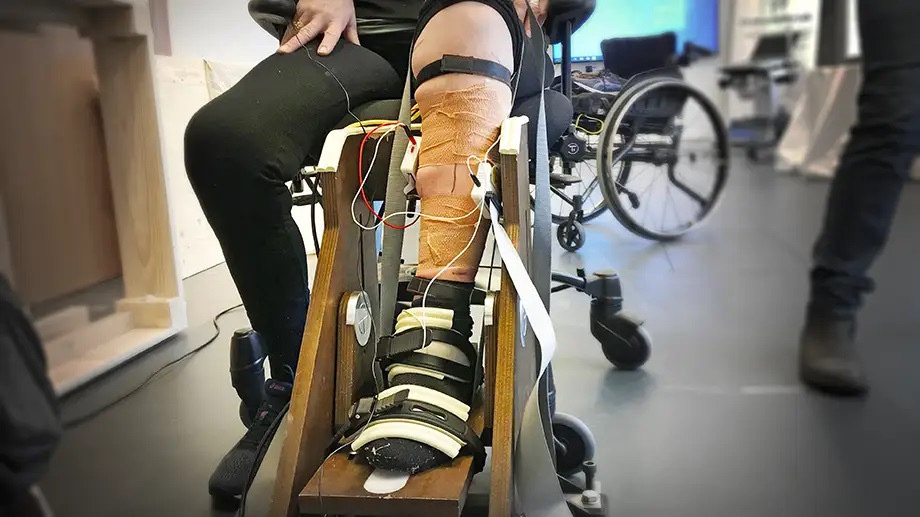
Even when people with incomplete spinal cord injuries can walk, everyday functions like standing, balancing or producing steady force may remain difficult. A new study shows why.
Using surface skin electrical sensors, a research team in Sweden identified previously unseen changes in motor coordination that result from incomplete spinal cord injuries (SCI). The study is the first to examine how individual motor units (nerve to muscle connections that create movement) work together in people with SCI.
“Our study reveals, at the cellular level, how the central nervous system adapts to the injury to control movement,” says Ruoli Wang, associate professor in biomechanics at Promobilia MoveAbility Lab, KTH Royal Institute of Technology. She says the researchers’ approach was completely non-invasive.
The results were published in the Journal of NeuroEngineering and Rehabilitation.
The study’s lead author, PhD student Zhihao Duan, says the researchers found the nervous system struggles to spread signals smoothly across muscles at low levels of exertion after the injury. And it appears to overcompensate at higher levels of exertion, sending “louder”, less refined signals.
Effect on motor units
Muscles move through hundreds or thousands of motor units, each turning on and off precisely to create smooth force. Composed of a single motor neuron and its connecting muscle fibres, these motor units respond to shared signals from the nervous system, much like different sections of musicians led by an orchestra conductor. That shared input is what allows them to act in coordinated patterns.
To explore how well these units coordinate under the control of the central nervous system, the team examined 25 people (including 10 control participants). They used high-density electromyography (HD-EMG) to measure electrical activity in the functionally similar calf muscles – soleus and gastrocnemius – while volunteers pushed lightly or moderately against a device.
Duan says that at 20% effort, fewer of the motor units in the two calf muscles were working in a shared, coordinated way compared with people without injury. As a result, their movements were shaky and unstable. “They were much less being driven by the same coordinated signal from the nervous system.” he says.
At a higher level of effort (50%) the SCI group showed stronger lowfrequency synchronization between the two muscles. The body loses flexibility and precision in control of the movement. “This could be a sign of the nervous system compensating by sending louder, less refined signals,” Duan says.
Unique insights
“One interesting finding is that after spinal cord injury the nervous system becomes more rigid and less able to change its approach as the muscles work harder. A healthy nervous system on the other hand is able to adapt its strategy as force demands, to adjust the shared neural drive level,” Wang says.
Although the study was limited by a small sample size and challenges in identifying enough motor units per muscle from the skin surface, Wang says the results offer unique insight into how SCI reshapes motor control.
“This finding may open the door to a new rehabilitation biomarker, helping clinicians and researchers design new neurorehabilitation strategies to re-tune the spinal cord control and to restore coordinated neural input,” she says.