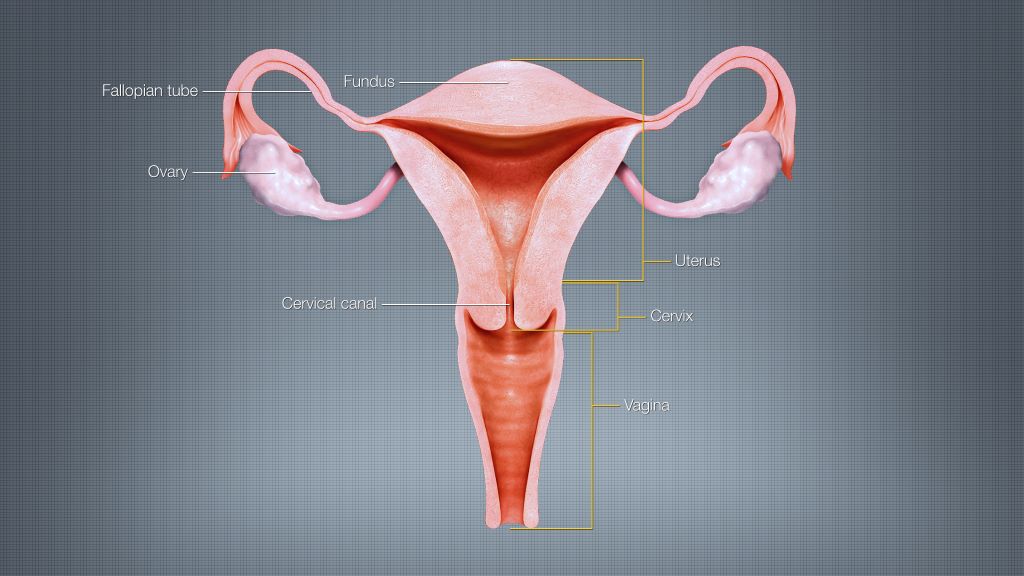
Fish During Pregnancy – What’s Safe, What’s Not?

Fish consumption during pregnancy is a complex scientific topic. While fish are rich in nutrients essential to brain development, such as polyunsaturated fatty acids, selenium, iodine, and vitamin D, they also contain methyl mercury, a known neurotoxicant. This has led the US Food and Drug Administration to recommend that expectant mothers limit consumption, inadvertently causing many women to completely stop eating fish during pregnancy.
Fish consumption is an important route of methyl mercury exposure, however, efforts to understand the health risk posed by mercury are further complicated by the fact that the nutritional benefits from fish may modify or reduce the toxicity posed by mercury. A new study appearing in the American Journal of Epidemiology based on data from a cohort of residents of a coastal community in Massachusetts creates a new framework that could untangle these questions, reduce confusion, and produce clearer guidance on fish consumption for pregnant mothers.
“We propose an alternative modelling approach to address limitations of previous models and to contribute thereby to improved evidence-based advice on the risks and benefits of fish consumption,” said the authors. “In fish-eating populations, this can be addressed by separating mercury exposure into fish intake and average mercury content of the consumed fish.”
The new research comes from an analysis of data from the New Bedford Cohort, which was created to assess the health of children born to mothers residing near the New Bedford Harbor Superfund site in Massachusetts. The current study included 361 children from the cohort who were born between 1993 and 1998 and at eight years old, underwent neurodevelopment assessments, including tests for IQ, language, memory, and attention.
The researchers were able to measure mercury exposure during the third trimester of pregnancy through hair sample collected from the mothers after birth. While hair samples have been the traditional method to study maternal mercury exposure, this approach alone cannot distinguish between mothers who frequently consumed low-mercury fish compared to those who consumed a smaller quantity of high-mercury fish.
To overcome this limitation, the researchers instead created a model that includes estimates of mercury exposure per serving of fish. This was possible because mothers in the cohort also completed a food questionnaire and reported the type and frequency of fish and shellfish consumed during pregnancy. The authors estimated the average mercury levels by type of fish, and when combined with the information about the mother’s diet, they were able to create a more precise and detailed method to estimate the joint associations of pregnancy fish intake and fish mercury levels on neurodevelopment.
Using this model, the researchers found that the relation between pregnancy fish consumption and subsequent neurodevelopment varied depending on the estimated average mercury levels in the fish. Specifically, consuming low mercury-containing fish was beneficial, while consuming fish with higher levels of mercury was detrimental.
“Given methodologic limitations to previous analyses, future work expanding our alternative modelling approach to account for both the average mercury and nutritional content of fish could facilitate better estimation of the risk-benefit tradeoffs of fish consumption, a key component of many healthy diets,” said the authors.
The authors are in the process of applying this model to other large studies of maternal fish consumption, including the Seychelles Child Development Study.