Flawed Advice on Drug Safety is Pushing Women to Stop Breastfeeding – New Study
The evidence supporting the health benefits of breastfeeding is overwhelming, yet many women taking medicines are advised to stop, often unnecessarily.

The evidence supporting the health benefits of breastfeeding is overwhelming, yet many women taking medicines are being advised to stop, often unnecessarily, according to a new study from the University of Bath.
The research, led by scientists in the Department of Life Sciences at Bath, reveals that concerns about drug safety during breastfeeding are a significant factor in the decision to stop, yet many medications prompting women to stop breastfeeding have either been found to cause no harm in limited studies, or the potential risks to the infant are considered minimal and outweighed by the benefits to the mother.
The new study, published today in the International Breastfeeding Journal, found that up to 18% of women who need a medication stopped breastfeeding due to that medication, rising to up to 58% among those with chronic illnesses.
These findings were supported by a Public Health England survey of 500 UK mothers, where 71% of respondents agreed with the statement, “It (breastfeeding) could prevent me from taking medication.”
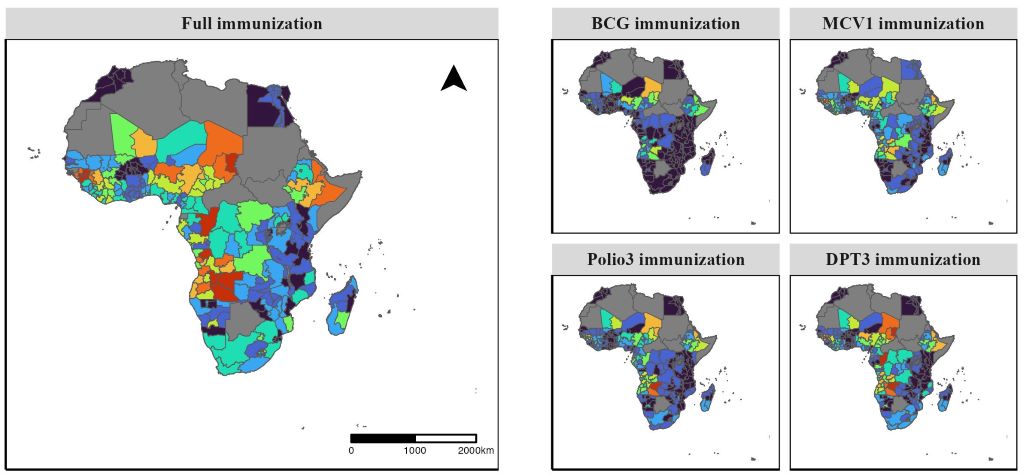
The Bath study reviewed research from seven countries across Europe and the USA spanning the past two decades. It was inspired by the researcher’s personal experience as a breastfeeding mother and pharmacist, which led her to undertake a PhD at the University of Bath.
“I suspected the advice I was getting wasn’t right,” said Rachel Pilgrim. “I felt quite nervous challenging the doctor – even though, as a pharmacist, it’s usually part of my job to do that, it felt very different as a patient. But the experience made me think – what it is like for women who don’t feel able to speak up?”
Breastfeeding is widely recommended by health authorities the world over. In the UK, exclusive breastfeeding is advised for the first six months of life, with continued breastfeeding alongside solid foods until at least one year.
Yet, despite widespread promotion of breastfeeding, the UK continues to report some of the lowest breastfeeding rates in Europe. While nearly half of mothers (49%) are breastfeeding at 6-8 weeks after giving birth, only 1% breastfeed exclusively to six months, according to a 2010 UK survey.
International surveys have found that exclusive breastfeeding at six months is reported in 27.2% of infants in the USA, 38% in Canada, and 37.5% in Australia.
The evidence gap
The maternal use of medication during breastfeeding does require caution, as some drugs can pass into breastmilk and affect the baby. However, for many medications, the amount transferred is minimal and unlikely to cause harm.
One problem lies in the lack of clinical trial data, as breastfeeding women are typically excluded from pharmaceutical trials due to the ethical implications of exposing a baby to an untested drug. Information on the effects of a medicine during breastfeeding builds slowly once a new drug starts to be used.
However, key medicines information resources for clinicians, such as the British National Formulary (BNF), often advise against drug use during breastfeeding, not because the medicine is definitely unsafe, but because its effects are not known with certainty. This conservative stance can lead to overly cautious or even incorrect advice. The study found that even for common medications such as antidepressants and painkillers – where safety data is well-established – women are stopping breastfeeding.
“The BNF is the first place most professionals look, but it doesn’t always reflect the full picture,” said Ms Pilgrim.
“As a result, the advice given to women is often incorrect. And even when the safety data is more limited, women need to be given accurate, balanced information that considers both the risks of the medication and the benefits of continued breastfeeding.”
Real-world impact
An evaluation of the Drugs in Breastmilk Service, run by the UK-based Breastfeeding Network, has found that 21% of mothers who contacted the service had been advised to stop breastfeeding by a healthcare professional. In 98% of these cases, this advice was found to be incorrect, and the women could have safely continued breastfeeding.
Alarmingly, fewer than 6% of these women were referred to the service by a healthcare provider – most found it through social media or peer support groups.
This disconnect between available evidence and clinical practice is contributing to unnecessary breastfeeding cessation, says Ms Pilgrim.
Both Ms Pilgrim and Dr Matthew Jones – who co-authored and supervised the study – are sympathetic towards clinicians who err on the side of caution when prescribing to breastfeeding mothers.
Dr Jones, an academic and pharmacist in the Department of Life Sciences at Bath, said: “Double checking the ‘conservative’ advice found in the BNF is highly time consuming.
“In my previous job as an NHS medicines information specialist, I might spend two hours verifying the safety of a drug using more specialist resources. Most people don’t have that kind of time.”
Study co-supervisor Dr Sarah Chapman from King’s College London, added: “We know breastfeeding women frequently choose not to take safe, beneficial medications because of misinformation and worries about effects on their baby; this study shows women also stop breastfeeding unnecessarily.”
Plans to improve safety awareness
Ms Pilgrim will build on her study through a three-phase PhD research project due to start in September and funded by Pharmacy Research UK.
As part of this work, she will develop a resource to make it easier for people to access specialist advice on breastfeeding. This will either be aimed at healthcare professionals or at women themselves.
Her goal is to improve communication between healthcare professionals and women, raise awareness that most drugs are safe to take when breastfeeding and ultimately support more women to continue feeding their babies while taking essential medications.
Source: University of Bath