Tamoxifen Found to be Ineffective in Fungal Meningitis Trial

In a disappointing outcome, a clinical trial has shown that tamoxifen, a promising candidate to improve survival for a deadly form of fungal meningitis, is ineffective. The trial was conducted by University of Oxford researchers and published in eLife.
The study finds that adding tamoxifen, a breast cancer drug, to standard antifungal treatment was no faster in clearing fungal infection from the spinal fluid of people with meningitis. More patients who received tamoxifen had evidence of heart conduction disturbances, rates of severe side effects were similar.
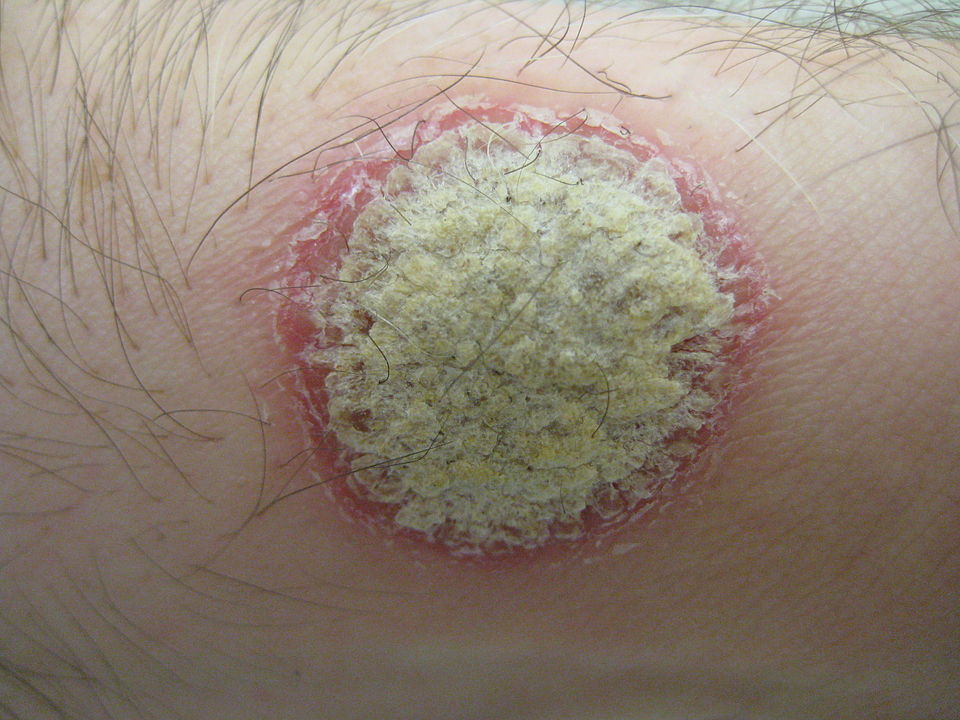
Cryptococcal meningitis is a leading cause of death in people with HIV, but also affects those without HIV, regardless of whether they are immunocompromised. Most infections are caused by a fungus called Cryptococcus neoformans (C. neoformans) and occur in low-income tropical settings. The gold-standard treatment is a combination of three drugs: flucytosine and amphotericin B initially, followed by fluconazole. Yet, even on this gold-standard therapy, a third of patients die within 10 weeks of being diagnosed. Moreover, the drug flucytosine is severely restricted by availability and cost, meaning it is rarely used where the disease burden is highest.
Co-first author Nguyen Thi Thuy Ngan, Clinician at the Oxford University Clinical Research Unit (OUCRU): ‘Tamoxifen has shown antifungal activity against various yeasts in the lab; we subsequently showed that it acts synergistically with amphotericin against two-thirds of clinical Cryptococcus isolates from our archive. As a well-understood, off-patent, cheap and widely available medicine, it was a promising candidate for treating cryptococcal meningitis.’
Co-first author Nhat Thanh Hoang Le, Biostatistician at OUCRU, added: ‘We designed a randomised trial to determine whether using these drugs in combination could improve the speed of clearance of Cryptococcus from patients with meningitis with and without HIV.’
The trial involved 50 patients, 40 with HIV. Of the patients, 24 were assigned to receive a standard anti-fungal treatment of amphotericin B and fluconazole plus tamoxifen, and 26 received the standard anti-fungal treatment only. Researchers measured the Early Fungicidal Activity (EFA) for both groups – how quickly C. neoformans amounts declined in a patient’s spinal fluid in the two weeks following treatment.
Based on their prior work, the team were hoping for better EFA for patients receiving tamoxifen, but there was no detectable difference in EFA.
The only observed difference was increased heart toxicity in the tamoxifen group. Lab studies had shown that a tamoxifen dose five to 10 times higher than that used routinely in breast cancer would be needed to have an antifungal effect. However, high doses of tamoxifen cause QT prolongation, which can cause cardiac arrest. While there was one sudden death in the tamoxifen group in this study, this occurred after the period of tamoxifen administration and it was not associated with an abnormal heart rhythm.
Senior author Professor Jeremy Day, Professor of Infectious Diseases, Oxford University, said: “Despite its apparent anti-cryptococcal effect and synergy with other drugs, tamoxifen does not increase the rate of clearance of yeast from spinal fluid in people with meningitis and is unlikely to result in clinical benefit.
“Our results show the importance of small-scale trials such as this for rapidly evaluating repurposable drugs and preventing the time and cost of a larger clinical study that is likely to fail. However, sadly this does mean that we urgently still need new, specific anti-cryptococcal drugs to be developed, and we also need to ensure that existing, available treatments are made accessible and affordable.”
Source: Oxford University