A New Treatment for Chronic Tendon Disease
The Achilles tendon can endure a load nearly 8 times body weight during exercise, rendering it vulnerable to injury despite its strength, which can be worsened by a failure to properly heal, forming bone instead of new tendon. A new study found that by inhibiting blood vessel formation, the anomalous bone growth can be prevented.
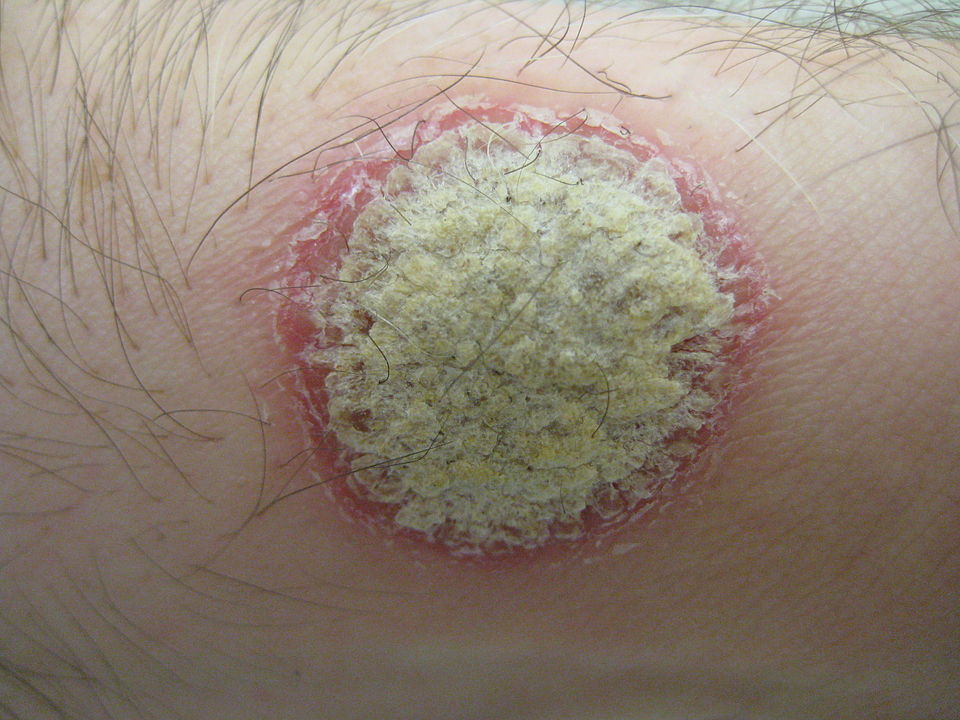
Due to the unique nature of tendons, failing to consult a doctor soon after an injury can lead to chronic tendon disease, which is characterised by pain, swelling, and movement problems. Tendon heterotopic ossification (HO) is a rare type of chronic tendon disease where new bone grows the tendon, causing even more damage. Famous athletes have had to retire early from sports due to a lack of a radical solution for Achilles tendon injuries.
Using single-cell sequencing technology, a team led by Professor Ouyang Hongwei found that changes in the tissue microenvironment of tendon HO alterations in gene expression and in tendon stem progenitor cells. These findings were published in Bone Research, providing a novel treatment for tendon heterotopic ossification.
The researchers firstly found that the tendon specific transcription factor MKX decreased significantly in heterotopic ossified human tendon, and deletion of MKX led to spontaneous ossification of mouse tendon, suggesting that MKX plays a critical role in tendon HO.
Further studies revealed that MKX knockout mouse tendon cells expressed high levels of genes related to blood vessel formation, resulting in vascular invasion and remodelling of the tendon extracellular matrix. This also resulted in abnormal activation of genes related to bone and cartilage in tendon stem cells. These data indicated that inhibition of blood vessel formation may improve the tendon tissue microenvironment and prevent HO progression.
Armed with this knowledge, Prof Ouyang and his colleagues searched for drugs that can inhibit the angiogenesis process. They found that local injection of a small molecule inhibitor known as BIBF1120 significantly inhibited the neovascularisation of tendon after injury, thus alleviating the progression of tendon HO.
Source: MedicalXpress