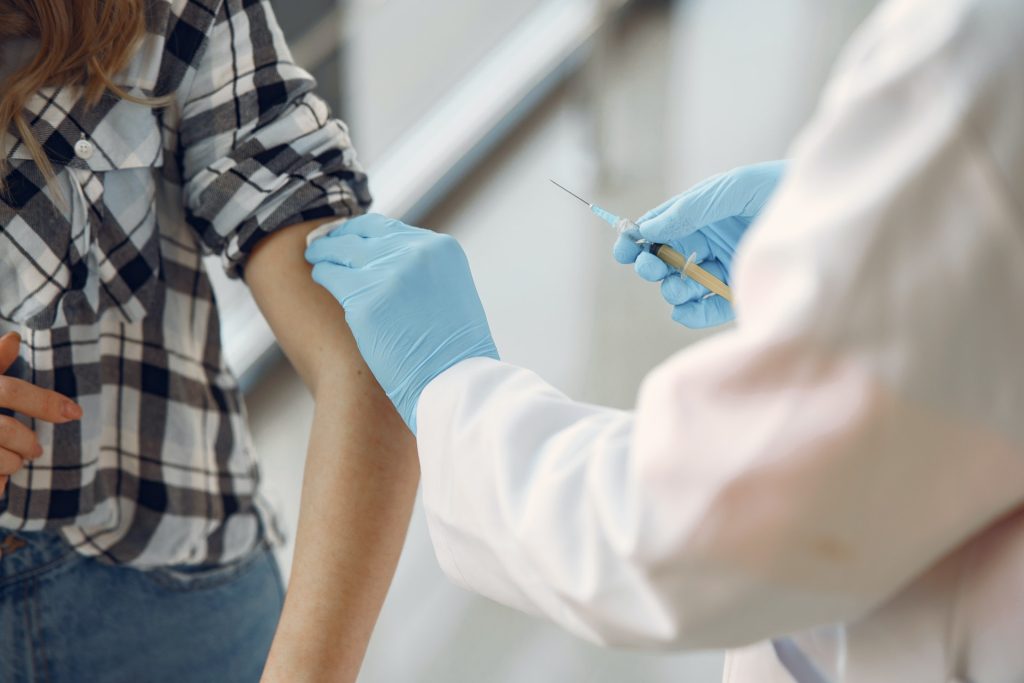
Distressed Individuals were Strong on COVID Vaccination but Lax on Social Distancing
During the COVID pandemic, individuals who were distressed, showing signs of anxiety or depression, were less likely to follow recommendations from the Centers for Disease Control and Prevention, yet they were more likely to get vaccinated than non-distressed peers.
The authors refer to this as differential distress: when people act safely in one aspect while disregarding safety in another, both in response to the same psychological distress. This creates a conundrum for those trying to determine how best to communicate risks and best practices to the public.
Their study of 810 people revealed that distress was less likely to affect older people either way, despite their higher risk for severe outcomes if infected with SARS-CoV-2. Reported in Frontiers in Psychology, the findings suggest that fear messaging, which is intended to scare people and can increase their levels of distress, may not be the most effective way to encourage people to change behaviours.
“These findings do not point to a straightforward public health messaging campaign,” said Professor Joel Myerson, study leader. “Instead, officials may have to consider more finely tailored messages for different populations in order to achieve best outcomes: more attention to CDC recommendations as well as more people getting vaccinated.”
In a previous study, the researchers looked at social distancing and hygiene behaviours across a range of demographics. The results suggested that distress was closely tied to the way people responded to recommendations about social distancing. People who were more distressed were less likely to observe social distancing recommendations, perhaps as a way to maintain social connections that can ease anxiety and depression.
In the latest work, researchers again asked people about their adherence to the latest CDC recommendations, including newer recommendations outlining when to wear a mask and suggesting that people avoid spending lots of time inside with others. The results showed similar correlations to the previous study among age, distress and behaviour changes.
In terms of public health and effective messaging, one of the most pressing issues to arise after publication of the first study was the introduction of vaccines and the perceptions around them. Looking at four categories, fully vaccinated; partially vaccinated; unvaccinated but likely to get one; unvaccinated and unlikely to get one, researchers found:
- People who had been fully vaccinated were more likely than those who were partially vaccinated to have close interactions with others following their shots.
- Relative to those who said they were unlikely to get vaccinated, those who said they were likely to do so thought their chance of infection was higher.
- Depending on the person’s age, they responded differently to the same level of stress. Overall, for example, the higher level of distress someone had, the less likely they were to social distance, but the more likely they were to get vaccinated. Both of these correlations became weaker, however, as people aged.
Fear messaging that tries to scare people into following guidelines tends to be useful only for a one-time event, Green said. “Ostensibly, getting vaccinated should count as such an event.” But as breakthrough cases increase and boosters add up, vaccinations are no longer one and done; they are instead a series of events, spread out over more than a year.
Although fear-based messaging may encourage younger people to get vaccinated, it also weakens their resolve to mitigation behaviours like social distancing. Not doing both poses a greater breakthrough infection risk.
Messaging also becomes less effective as people age, just as they become more vulnerable to severe illness.
“Part of the solution to the problem of differential distress may be to avoid the distress altogether,” said Professor Leonard Green, study co-lead. This would entail forgoing the fear campaign. Instead, a gentler approach may be warranted. “Our previous work suggests that what really motivates many people to change behaviours for the better is considering how their actions can benefit, or harm, other people.”