Metformin for Gestational Diabetes may Negatively Impact Offspring

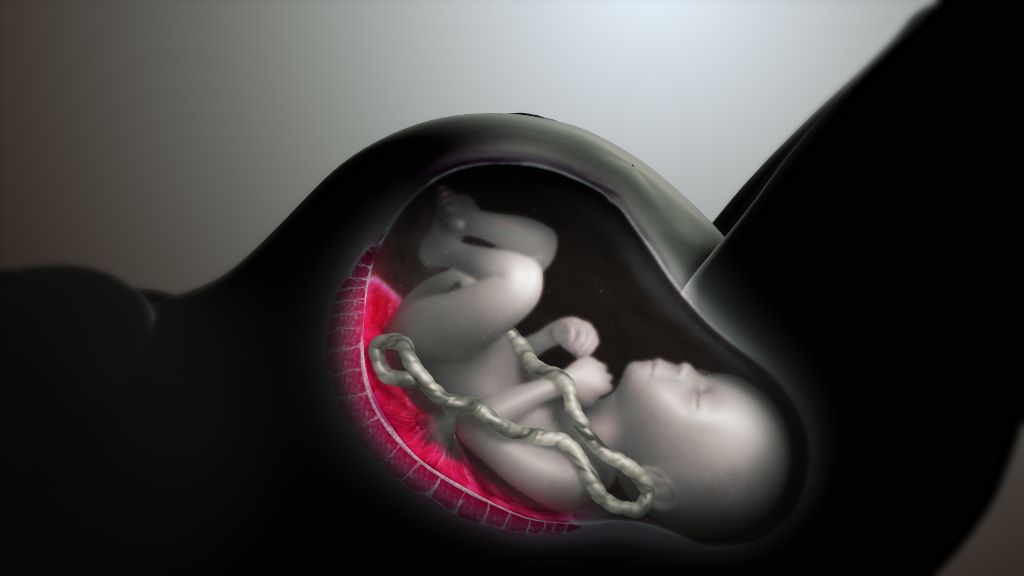
With the rise in gestational diabetes and metabolic disorders during pregnancy, metformin is also being prescribed more frequently. Although it is known that the oral antidiabetic agent can cross the placental barrier, the impacts on the brain development of the child are largely unknown. Now, researchers have been able to demonstrate in a mouse model that although metformin has positive effects in pregnant animals, it does not in the offspring. The researchers, from German Institute of Human Nutrition Potsdam-Rehbrücke (DIfE), published their findings in Molecular Metabolism.
Around one in six pregnant women worldwide are affected by gestational diabetes. According to the Robert Koch Institute, 63 000 women in Germany were affected by the disease in 2021, and the trend is increasing. Excessively high blood sugar levels during pregnancy are associated with negative consequences for mother and child. It increases the risk of affected women developing type 2 diabetes later on and their children have a higher risk of developing metabolic disorders and being overweight.
Long-term effect of metformin on offspring is unclear
The placenta-crossing oral antidiabetic agent metformin has been gaining importance as an alternative to insulin administration when lifestyle changes fail to treat gestational diabetes. But there are currently only a few studies on the long-term effects of metformin on the health of offspring. It is known that metformin has an impact on the AMPK signaling pathway, which regulates the networking of nerve cells during brain development.
The interdisciplinary team of DIfE researchers led by Junior Research Group Leader Dr Rachel Lippert therefore grappled with two central questions:
Firstly, is metformin treatment only beneficial for the mother or also the child?
Secondly, does metformin treatment lead to long-term negative physiological changes in the offspring, especially in connection with the development of neuronal circuits in the hypothalamus, a critical region in the regulation of energy homeostasis?
Mouse models shed some light
To answer the key questions, the researchers used two mouse models with high-fat or control diets to represent the main causes of gestational diabetes, ie, severe obesity of the mother before pregnancy and excessive weight gain during pregnancy. The antidiabetic treatment of female mice and their offspring took place during the lactation period as this corresponds to the third trimester of a human pregnancy in terms of brain development.
The mice were treated with insulin, metformin, or a placebo, with dosage based on standard human treatments. The research team collected data on the body weight of the mice, analysed various metabolic parameters and hormones, and examined molecular signaling pathways in the hypothalamus.
Maternal metabolic state is crucial
“As a result of antidiabetic treatment in the early postnatal period, we were able to identify alterations in the weight gain and hormonal status of the offspring, which were critically dependent on the metabolic state of the mother,” explains Lippert. Furthermore, sex-specific changes in hypothalamic AMPK signalling in response to metformin exposure were also observed. Together with the metformin-induced shift in the examined hormone levels, the results indicate that the maternal metabolic state must be taken into account before starting the treatment of gestational diabetes.
Focusing on prevention
According to Rachel Lippert, treatment of gestational diabetes in future could entail developing a medication that is available for all and does not cross the placenta. “Given the increasing prevalence, education about gestational diabetes and preventive measures are of vital importance. If we can find a way to manage lifestyle and diet more proactively, we are in a better position to exploit the potential of gestational diabetes treatment,” says Lippert.