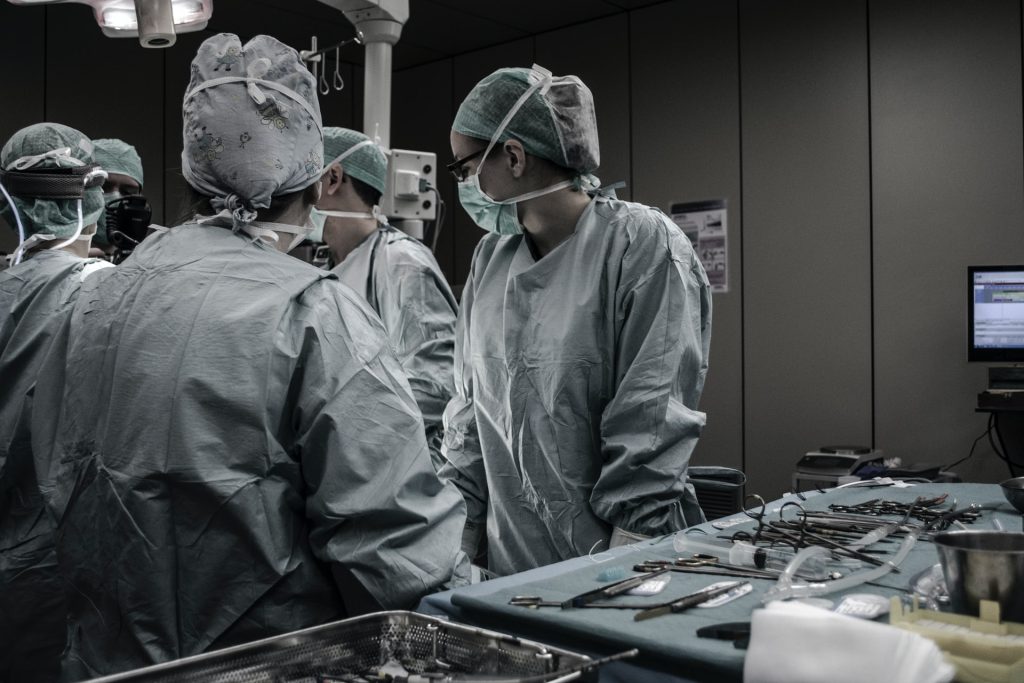
Nearly Half of Female Surgeons Experience Pregnancy Complications

A survey of female surgeons found that 48 percent had experienced major pregnancy complications, with even higher risks for those with more operation hours per week in the last trimester of pregnancy.
Women are entering the surgical field in increasing numbers but they continue to face well-known challenges related to childbearing. Surveys have documented pregnancy-related stigma, unmodified work schedules, brief maternity leave options, and little support for childcare and lactation needs after delivery. Due to a lack of childcare options in developed countries, many female trainees delay pregnancy until after 35, already a risk factor for pregnancy complications, researchers from Brigham and Women’s Hospital and elsewhere surveyed 1175 surgeons and surgical trainees from across the US to study their or their partner’s pregnancy experiences. They found that 48 percent of surveyed female surgeons experienced major pregnancy complications, with those who operated 12-or-more hours per week during the last trimester of pregnancy at a higher risk compared to those who did not. Their findings are published in JAMA Surgery.
“The way female surgeons are having children today makes them inherently a high-risk pregnancy group,” said corresponding author Erika Rangel, MD, MS, of the Division of General and Gastrointestinal Surgery. “In addition to long working hours, giving birth after age 35 and multiple gestation which is associated with increased use of assisted reproductive technologies – is a risk factor for having major pregnancy complications, including preterm birth and conditions related to placental dysfunction.”
The researchers found that over half (57 percent) of female surgeons worked more than 60 hours per week during pregnancy. Over a third (37 percent) took more than six overnight calls. Of the 42 percent of women who experienced a miscarriage (a rate twice that of the general population) three-quarters took no leave afterwards.
“As a woman reaches her third trimester, she should not be in the operating room for more than 12 hours a week,” Dr Rangel said. “That workload should be offset by colleagues in a fair way so that it does not add to the already-existing stigma that people face in asking for help, which is unfortunately not a part of our surgical culture.”
Male and female surgeons were asked to respond to the survey, which had been developed with obstetricians and gynaecologists. Nonchildbearing surgeons answered questions regarding their partners’ pregnancies. The investigators found that, compared to female nonsurgeons, female surgeons were 1.7 times more likely to experience major pregnancy complications, along with greater risk of musculoskeletal disorders, non-elective caesarean delivery, and postpartum depression, which was reported by 11 percent of female surgeons.
“The data we have accumulated is useful because it helps institutions understand the need to invest in a top-down campaign to support pregnant surgeons and change the culture surrounding childbearing,” Dr Rangel said. “We need to start with policy changes at the level of residency programs, to make it easier and more acceptable for women to have children when it’s healthier, while also changing policies within surgical departments. It is a brief period of time that a woman is pregnant, but supporting them is an investment in a surgeon who will continue to practice for another 25 or 30 years.”
Source: Brigham and Women’s Hospital
Journal information: Rangel EL et al. “Incidence of Infertility and Pregnancy Complications in US Female Surgeons” JAMA Surgery DOI: 10.1001/jamasurg.2021.3301