Scientists Discover a Form of Constipation Caused by Gut-drying Bacteria
Two bacteria working together to break down intestinal mucus are identified as a contributing factor to chronic constipation
Scientists at Nagoya University in Japan have found two gut bacteria working together that contribute to chronic constipation. The duo, Akkermansia muciniphila and Bacteroides thetaiotaomicron, destroy the intestinal mucus coating essential for keeping the colon lubricated and faeces hydrated. Their excess degradation leaves patients with dry, immobile stool. This discovery, published in Gut Microbes, finally explains why standard treatments often fail for millions of people with chronic constipation.
Notably, the study shows that Parkinson’s disease patients, who suffer from constipation decades before developing tremors, have higher levels of these mucus-degrading bacteria. While constipation in Parkinson’s disease has traditionally been attributed to nerve degradation, these findings suggest that bacterial activity also plays a crucial role in the development of their symptoms.
Why mucin matters for digestion
Constipation is a very common digestive problem. Doctors have assumed it happens because of slow gut movement when our intestines are not moving food along fast enough. However, this explanation does not work for everyone.
Some people have constipation with no identifiable cause, referred to as chronic idiopathic constipation (CIC). Parkinson’s disease patients also face severe, treatment-resistant constipation, though it is clinically categorized separately from CIC. Many struggle with severe constipation for 20 or 30 years before they develop tremors and movement problems, but researchers did not know why until now.
Instead of focusing on nerve and muscle movement in the gut, the researchers examined the protective gel-like coating called colonic mucin, a substance in the large intestine that lines the intestinal walls and is found within stool. Colonic mucin keeps stool moist, helps it move smoothly through our digestive tract, and protects the intestinal wall from bacteria.
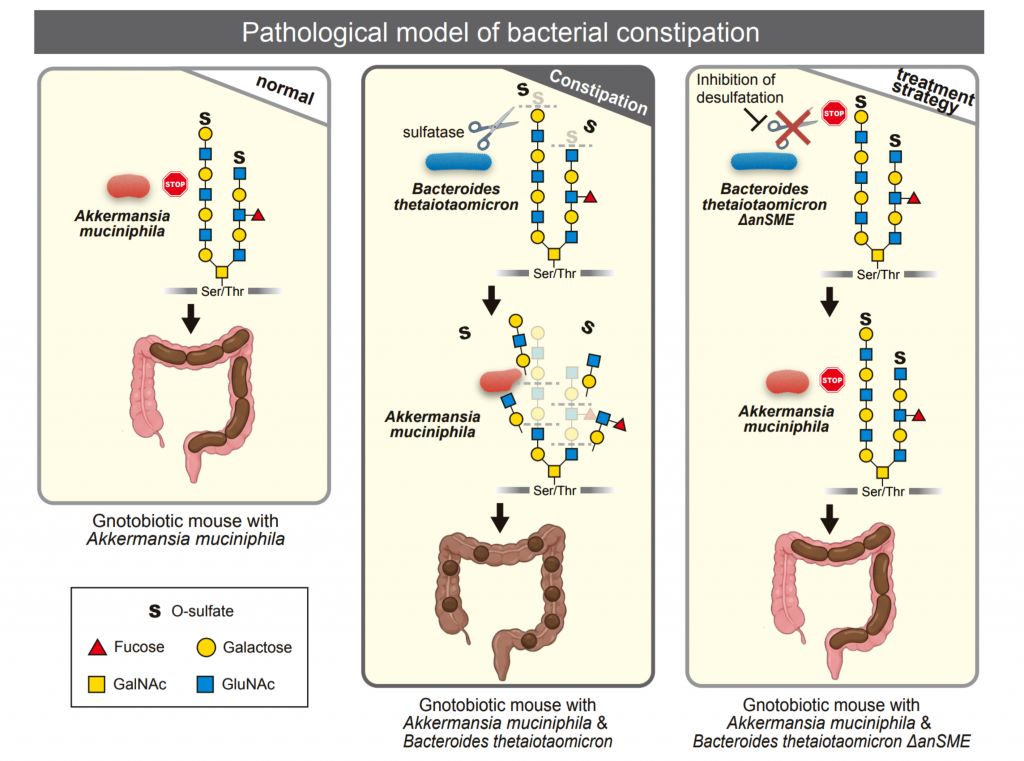
They found that two gut bacteria work in sequence to break down this mucin. B. thetaiotaomicron uses enzymes to remove protective sulfate groups from the mucin, and A. muciniphila then breaks down and consumes the exposed mucin.
Sulfate groups attached to colonic mucin molecules normally prevent bacteria from degrading them. When too much mucin is destroyed, stool loses moisture and becomes hard and dry, causing constipation. Because the problem is mucin loss, not slow gut movement, standard laxatives and gut motility drugs are often ineffective.
A new frontier for gut health treatment
“We genetically modified B. thetaiotaomicron so it could no longer activate the enzyme sulfatase that removes sulfate groups from mucin,” Tomonari Hamaguchi, lead author and lecturer from the Academic Research & Industry-Academia-Government Collaboration Office at Nagoya University explained.
“We put these modified bacteria into germ-free mice together with Akkermansia muciniphila, and surprisingly the mice did not develop constipation; the mucin stayed protected and intact.”
The experiment proved that blocking the sulfatase enzyme prevents the bacteria from degrading mucin. Therefore, drugs that block sulfatase could treat bacterial constipation in humans.
For millions of patients with treatment-resistant constipation, including those with Parkinson’s disease, this discovery offers hope for new therapies that address the root microbial causes of their condition.
Source: Nagoya University


