Closing the Gap on Eye Care Through Early Detection this World Optometry Week
Uneven access to optometry services in South Africa puts pressure on prevention, but collaboration and technology are helping shift the dial.

Access to good eye care in South Africa remains uneven, resulting in many conditions being diagnosed too late. World Optometry Week, observed from 22 to 28 March, shines a light on this reality, where one in 10 South Africans suffers from some form of vision loss, highlighting the importance of eye health and the role early detection plays in preventing avoidable vision loss.
This challenge is exacerbated by the fact that, while there are approximately 4 200 registered optometrists in South Africa, only a small proportion practise in the public sector. This limits access to care for many communities and delays diagnosis, particularly in under-resourced areas. As a result, prevention remains one of the most important, yet underutilised, tools in protecting eye health.
“The reality is that many serious eye conditions develop without noticeable symptoms early on,” says Dr Themba Hadebe, Clinical Executive at Bonitas. “By the time vision is affected, the condition may already be advanced. Regular eye tests are critical in detecting issues early and preventing avoidable vision loss.”
This year’s World Optometry Week theme, “A Shared Vision: Collaboration in Global Eye Care”, underscores the need for a coordinated approach to improve access, strengthen prevention and enable early diagnosis. This is one way to ease pressure on the broader healthcare system, since identifying conditions earlier reduces the likelihood of more complex interventions later, benefiting both patients and providers.
Why early detection matters
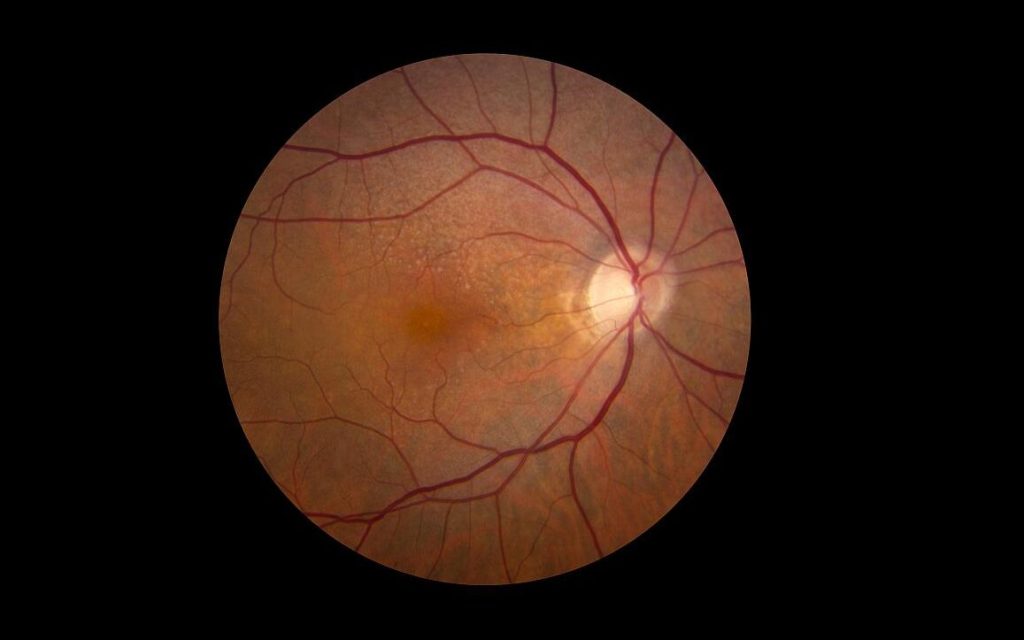
Conditions linked to chronic illnesses, particularly diabetes, remain a significant contributor to vision loss in South Africa. Diabetic retinopathy is among the leading causes of blindness in working-age adults, yet it often develops without pain or early warning signs.
Advances in optometric technology are beginning to shift how the risks of permanent damage are identified and managed. Developments highlighted by the American Optometric Association point to a growing role for AI-assisted diagnostics and enhanced imaging in improving both the speed and accuracy of screening. These tools support clinicians by flagging potential abnormalities during routine eye tests, enabling earlier referral for further assessment where needed.
Within this context, collaboration between medical schemes and provider networks plays a role in strengthening preventative care. Through its partnership with PPN, Bonitas provides members with access to diabetic retinopathy screening as part of the eye testing process at participating network practices.
The screening process uses AI-assisted technology to evaluate retinal images in real time, flagging any irregularities that could indicate early-stage disease. This allows clinicians to identify potential issues ranging from diabetic retinopathy to glaucoma or macular degeneration before they progress to more serious stages. Patients who require further assessment are referred for secondary care, ensuring timely intervention and reducing the risk of irreversible vision loss.
“This approach extends the reach of early detection by combining advanced technology with coordinated care and helps make the most of the limited number of specialists available,” says Hadebe. “Spotting problems early dramatically improves outcomes while reducing pressure on our healthcare system. In practice, it means a member could walk into a routine check-up and leave with peace of mind, or if something is flagged, a clear path to treatment.”
As World Optometry Week highlights, awareness must translate into action. In a healthcare environment where access is not equal, regular eye tests, particularly for those at higher risk, remain essential to safeguarding vision and improving long-term health outcomes.