TENS Shown to Improve Pain and Fatigue in Fibromyalgia
Real-world trial finds long-lasting benefit for TENS with physical therapy in reducing movement pain, fatigue
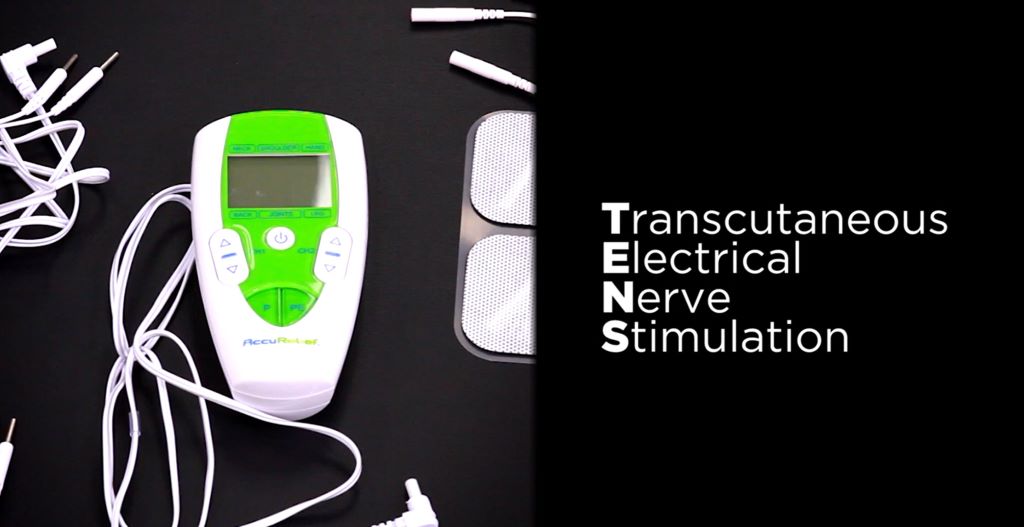
Adding TENS (transcutaneous electrical nerve stimulation) to outpatient physical therapy reduced movement-based pain and fatigue in patients with fibromyalgia, and the effects lasted for at least six months, according to a new study led by researchers at University of Iowa Health Care.
The study, led by Kathleen Sluka, PT, PhD, is the first real-world trial of TENS for fibromyalgia. The findings, published on March 27 in the journal JAMA Network Open, show that TENS is a safe, effective, inexpensive, and readily available treatment for fibromyalgia, a chronic condition that causes pain, tenderness, and fatigue throughout the body.
“It is one of the few treatments that specifically targets movement-evoked pain and fatigue, which are major barriers to participation in daily activities,” says Sluka, UI professor of physical therapy and rehabilitation science.
TENS uses a small device with adhesive electrodes to send mild electrical pulses through the skin to block or reduce pain. The study found that the effect of TENS for reducing pain was similar, if not better, than current FDA-approved medications for fibromyalgia.
“We were excited to see that patients also had less fatigue,” Sluka added. “Right now, there are no good treatments for fatigue. So, the fact that we had anything that touched the fatigue was pretty powerful.”
Fibromyalgia: complicated, misunderstood, and hard to treat
Fibromyalgia affects about 4% to 7% of the population. It significantly impacts a person’s physical function, cognitive abilities, and sleep. In addition to chronic pain, a key feature of the condition is whole-body fatigue, which interferes with day-to-day life and contributes to patients’ inability to concentrate and perform functional activities.
Exercise is often the first line of treatment recommended to people with fibromyalgia, and research has shown that it can be beneficial. However, fibromyalgia causes fatigue and pain, which is a key reason why the research team focused on alleviating pain with movement.
“Pain with movement hinders a person’s ability to participate in an effective exercise program and do their day-to-day activities.” Sluka says.
Science translated to real-world benefit
Sluka and her colleagues have spent decades studying the biological mechanisms affected by TENS, developing the ideal parameters of TENS stimulation and testing the efficacy of TENS for treating chronic pain and fatigue in human trials.
They have previously shown that under the ideal conditions of a randomized, controlled clinical trial, TENS in conjunction with physical therapy can significantly decrease movement pain.
The new Fibromyalgia TENS in Physical Therapy (FM-TIPS) study was designed to test the effect of TENS under real-world conditions. The study was conducted in 28 outpatient physical therapy clinics across six health care systems in the Midwest, and included 384 people of different ages, education levels, and socioeconomic backgrounds. Almost 50% of the participants were from rural areas.
“It was a challenge to recruit participants for this study, but the clinics and the physical therapists we worked with were great. This would never have happened without them,” Sluka says.
The clinics were randomised to provide either physical therapy (PT) with TENS or physical therapy alone. In the PT-TENS group, participants were asked to use TENS for two hours a day for six months. That time could be split into short periods or done all at once. The TENS electrodes were placed on the upper and lower back and delivered a mixed frequency signal at an intensity as strong as the participant could tolerate.
After 60 days, movement-evoked pain during TENS treatment was significantly improved in the PT-TENS group. Adding TENS also significantly reduced resting pain and resting and movement-fatigue. In contrast, participants who received only physical therapy had no change in their movement-evoked pain.
When we gave the PT-only patients the TENS unit and they started using it, we also saw the same improvements as the PT with TENS patients, which is powerful. – Kathleen Sluka, PT, PhD
The response also was dose-dependent, with people who used TENS daily for 60 days having the best outcomes.
Unlike many pain-relieving drugs that can become less effective over time as the body develops a tolerance for the medication, the study shows that over time, TENS maintained its ability to improve pain and fatigue at a significant level.
After the primary endpoint at day 60, the PT-only group was also given TENS, and all the participants continued in the study for another four months.
“When we gave the PT-only patients the TENS unit and they started using it, we also saw the same improvements as the PT with TENS patients, which is powerful,” Sluka says.
Overall, the study showed that 80% of patients found TENS helpful. At six months, 80% were still using TENS once a week, and over 70% reported they felt better after using TENS.
TENS adds benefit
Dana Dailey, PT, PhD, UI assistant research scientist and the first author of the study, notes that it’s important for people to realize that the benefit of TENS comes from using it as a part of a total treatment plan that includes physical therapy.
“Using TENS on its own will not give the same benefits,” Dailey says. “However, the study shows that TENS provides an added benefit on top of any relief from other treatments. All the study participants were also using pain medications and receiving physical therapy, yet TENS still provided additional relief.”
Fibromyalgia often needs multiple interventions to help patients feel less pain and fatigue and improve their overall function. The new findings suggest that TENS could be particularly helpful as a part of a multipronged approach because it can be safely and easily used as a self-management tool that uniquely targets movement-associated pain and fatigue.
“Often, when you move a randomised, controlled clinical trial into a real-world setting, it doesn’t work because there are too many confounding factors. But this intervention still works,” Sluka says. “Not only did the treatment reduce movement pain and fatigue during the testing period, but patients continued to use it at six months.”
Source: University of Iowa



