Timely Scan Could Save Lives of A&E Patients with Haematuria

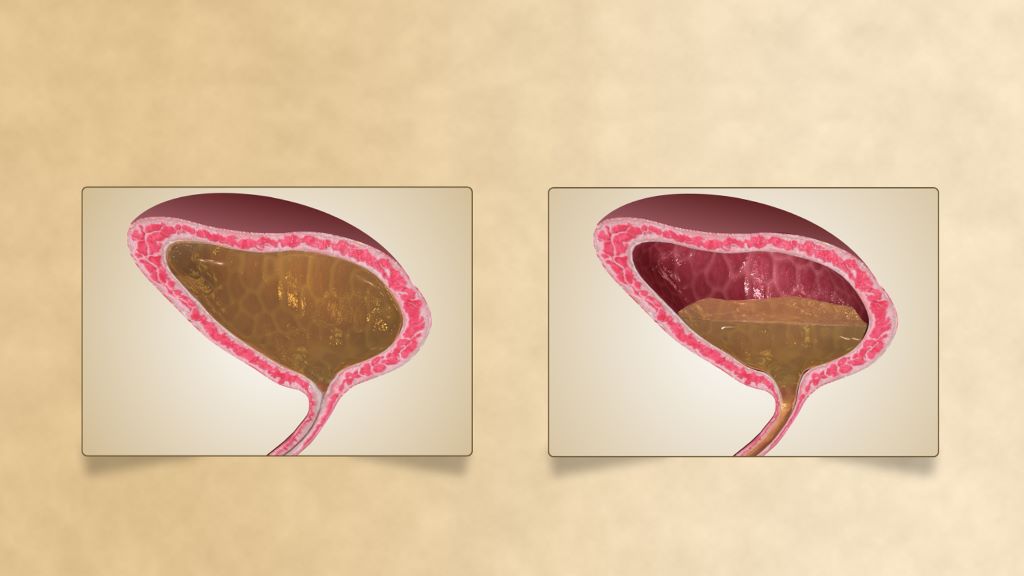
One in ten emergency patients with visible blood in their urine die within three months of presenting at A&E, new research has found. The WASHOUT study, presented Monday 16 March at the European Association of Urology Congress (EAU26) in London, found that a scan within 48 hours could reduce this risk.
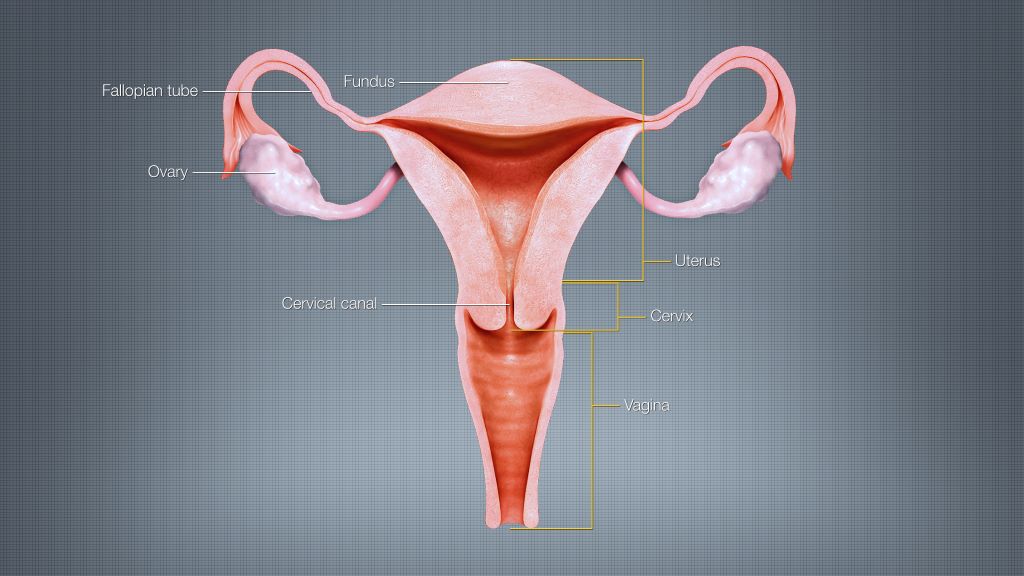
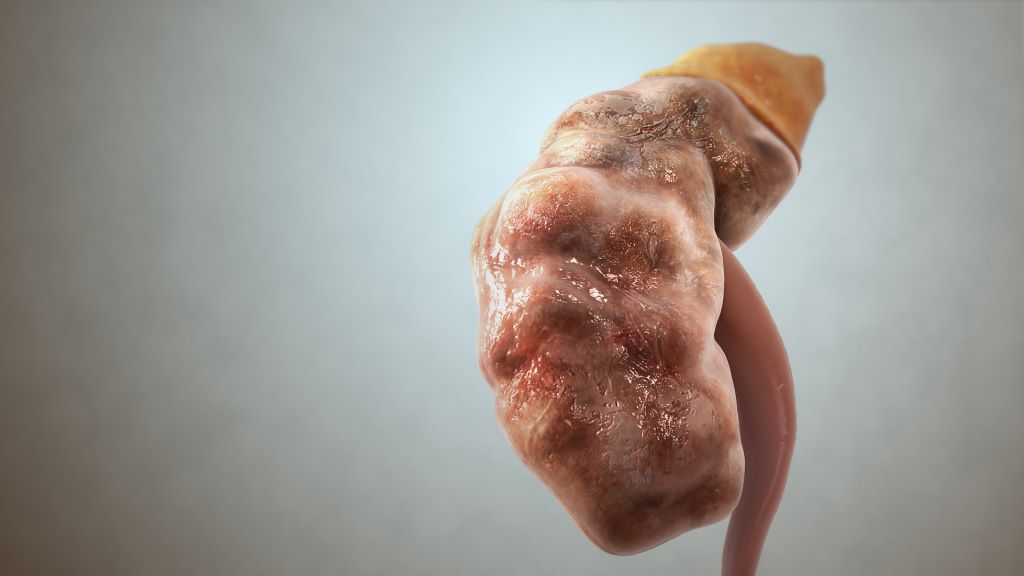
Such a scan also ensured patients with cancer were diagnosed significantly faster. Around 1 in 4 people who presented at A&E with visible blood in their urine had an underlying cancer, with the most common being bladder cancer, the study found.
Around 25 000 people visit UK A&E departments each year because they have blood in their urine. Currently, patients receive different care depending on which hospital they visit or even which doctor they see. This is because there are no guidelines built on real-world evidence for doctors to follow. Based on global figures, only around half (53%) of patients receive a scan and a third (35%) receive surgery, with others discharged home or admitted to the ward to watch how their symptoms progress, says the WASHOUT study.
The WASHOUT study drew on global data to show that rapid action is critical for better patient outcomes. A CT scan or cystoscopy to look inside the bladder within 48 hours of arriving at A&E should determine the most appropriate next steps – such as whether the person should be treated for bladder cancer. Patients who didn’t receive investigative tests or appropriate treatment were 2.5% more likely to die within the next three months compared to those who did. They also spent more time in hospital and were more likely to be readmitted with the same problem within three months.
For patients with an underlying cancer, those who received investigative tests within the first 48 hours of admission were diagnosed within one day on average. In contrast, patients who were discharged without investigation faced a significantly longer wait, with diagnosis taking on average three weeks.
The research team is now taking steps to incorporate their findings into clinical guidelines, to help hospital staff provide the best treatment for these patients.
The study looked at data from more than 8500 people across 380 hospitals around the world and followed their journey for 90 days after arriving at A&E with blood in their urine. It also considered other factors that might have affected results, including age, frailty and other underlying conditions.
Nikita Bhatt, consultant urologist at St Vincent’s University Hospital, Dublin, led the research being presented at EAU26. She said: “This is the largest study exploring how we should treat people who present at A&E with blood in their urine. It’s a common problem affecting thousands of people around the world, and these patients are usually very unwell. But too often they fall through the gaps because it isn’t obviously tied to a specific disease. Our findings show how important it is that doctors take the necessary steps to identify the cause of the problem. For patients, the message is clear: if you have visible blood in your urine, don’t ignore it. See your doctor as soon as you can. If it doesn’t clear up, keep pushing until you find an answer. I hope our study gives patients the encouragement to do that.”
Jacqueline Emeks, a patient advocate on the WASHOUT study, who was diagnosed with a kidney infection and sepsis after arriving at A&E with visible blood in their urine, agrees: “These findings highlight that blood in the urine should trigger immediate action. It’s not something to watch and wait. For patients, this should mean quicker triage, earlier investigations and faster treatment, translating into safer care, fewer delays, and a better chance of avoiding severe illness or long-term harm. Patients know their bodies and deserve to be taken seriously. Blood in urine is a red flag until proven otherwise.”
Prof Dr Joost Boormans, a member of the EAU Scientific Congress Office and a urologist at the Erasmus University Medical Center, Rotterdam, said: “This is an important study highlighting the scale of the problem that emergency blood in the urine presents, both for patients and our already over-stretched healthcare systems. It’s difficult to draw strong conclusions about specific conditions because blood in the urine can be caused by many things, including cancer, and this group of patients is very diverse. But this study shows that timely investigative tests can accelerate diagnosis and reduce patients’ risk of readmission and long hospital stays, both being significantly high as shown in the WASHOUT study. As urologists in emergency care, we should be aware of these numbers and do more to get an immediate diagnosis for people with blood in urine, to reduce the burden on our healthcare systems and give our patients the best outcomes.”
Source: European Association of Urology