In a leap for personalised medicine, scientists have discovered a simple and valuable way to improve brain cancer surgeries.
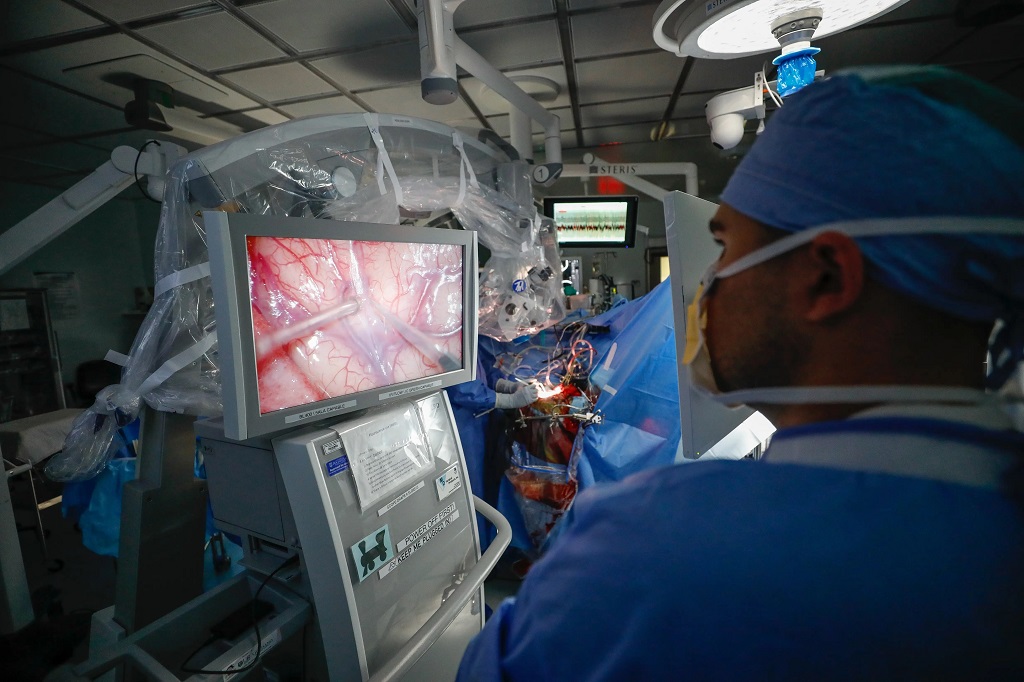
When removing cancerous tissue in the brain, neurosurgeons often use “awake brain mapping” to minimise the risk of causing unintended disruptions to a patient’s quality of life while removing as much tumour as possible. This practice, which has been used for decades, involves waking a patient up mid-surgery to test their neurocognitive functions in real time by stimulating the brain surface and assessing for functional changes.
A new study published in the journal Science Advances details a promising new avenue toward improving awake brain mapping results by investigating the tiny, nearly imperceptible variabilities in patient behaviour that occur during the procedure. This work, led by Carnegie Mellon University researchers, points to a future where brain surgeries are not just safer, but more precisely tailored to protect each patient’s speech, movement and quality of life.
How awake brain mapping works
As cancer grows in the brain, it rarely keeps to itself. Cancerous cells can be found in the seemingly healthy brain tissue surrounding a tumour, presenting neurosurgeons with a dilemma. They need to remove as much tissue infiltrated by cancer as possible, but they also need to avoid the removal of too much tissue since it can cause permanent harm to a patient’s ability to hold a fork or a conversation.
During awake brain mapping, surgeons gently stimulate the brain with small electrical impulses while the patient completes planned tasks. One of the most common applications of awake brain mapping is to identify where language is represented in a patient’s brain, which is done by having the patient name pictures or read words while their brain is being stimulated. If the patient can respond quickly and correctly, the clinicians know the part of the brain they stimulated can be safely removed. If the patient slurs or becomes unable to speak, then that part of the brain may be essential for language. Surgeons require a significant amount of experience to understand the nuances of this complex technique.
While the method may sound extreme, the brain has no sensory nerves, so patients do not feel their brain surgery as it is happening. Recent research also shows that for some types of brain cancer, improving a patient’s quality of life after surgery extends their expected survival into the future. This means that anything that can make awake brain mapping even more effective will translate into improved outcomes for brain cancer patients.
New measures show how slight changes in procedure affect patient behaviour
Based on a decade of research, the study authors uncovered new insights from examining the answers patients get wrong – and right – while undergoing awake brain mapping.
“We found that if you measure both the types of errors that patients make, as well as how fast they respond even when they do not make errors, more granular inferences can be drawn about language organization from an awake brain mapping procedure,” said Bradford Mahon, a cognitive neuroscientist at CMU’s Neuroscience Institute and Department of Psychology and senior author of the study. “We also found that physical parameters of the direct electrical stimulation delivered to the patient’s brain – such as its duration, and when it started and stopped relative to the task the patient is performing – were tightly related to small changes in patient behaviour that we could measure.”
Mahon and his team don’t yet know exactly what combination of parameters should be used to maximise the effect of direct electrical stimulation mapping. But they have discovered an intriguing signal hidden inside of the data that, until now, has gone unnoticed.
“What we have measured and formalised in our study is how slight changes in the awake mapping procedure can cause slight changes in patient behaviour. This is exciting because it is a new and meaningful signal that can be extracted from the data already being generated during awake brain mapping procedures,” said Mahon.
A new level of personalised medicine
The new study suggests that awake brain mapping may offer more informative and more personalized guidance for surgery than has been possible in the past.
“Stimulation has traditionally been treated as a binary test – either it causes an error, or it doesn’t,” said Raouf Belkhir, lead author and a psycholinguist who is completing the University of Pittsburgh-Carnegie Mellon University Medical Scientist Training Program. “But in reality, these effects are often more continuous than binary.”
For example, stimulating a particular area of the brain might reliably cause an error, never affect behaviour at all, or – more subtly – slow a patient’s response without causing an obvious mistake. In some cases, stimulation may affect behaviour at one moment, but not when tested again just seconds later.
“In other words, brain mapping isn’t always black or white,” said Belkhir. “Sometimes the most important information lives in the grey area.”
The nuance matters because every brain is different, which means every surgery is different, too. Understanding why stimulation has variable effects across different patients, and even within the same patient from one part of the surgery to another part of the surgery, may be key to protecting outcomes for future patients.
“Surgeons are seeking to optimise the balance between removing all of the cancerous tissue while preserving critical functions that may be represented by nearby brain regions,” said Mahon. “This research shows that by measuring aspects of patient performance that were previously not considered relevant for awake brain mapping, even better predictive models of brain organisation can be developed.”
If clinical teams have better predictive models personalised to each patient, then the consequences of different surgical approaches on postoperative neurocognitive function can be simulated. This allows for patients and their caregivers to personalise decisions to what is most important to the patient.
In other words, Mahon said, a business manager may consent to a surgery that may diminish their motor skills, but not their speech, whereas a concert violinist may prefer the opposite.
Bringing standardisation to awake brain mapping surgery
Another important development from this research is the startup company MindTrace, which has built an integrated software platform that supports neurocognitive testing before, during and after surgery. It is working to build a longitudinal dataset of patient outcomes that will be used to train forecasting models.
Tyler Schmidt, MD, study co-author and neurosurgeon at the University of Rochester, has used MindTrace in over a dozen awake surgeries since its release this year.
“In the beginning of brain tumour surgery, it used to be, ‘Can we remove any of this tumour safely?’” said Schmidt. ”But now in some brain tumour cases it’s, ‘Can we get you back to work potentially? Can we keep your quality of life close to what it was prior to your diagnosis? Can we hone in on the things that are most important to you and then try and protect them while getting the same oncological outcome?’” said Schmidt. “I think it’s a positive paradigm shift in how we take care of this patient population.”
The options today are measurably better than they were even 20 years ago. Clinicians now understand how to maximise the likelihood that patients have the best possible outcomes from brain cancer surgery.
“Ultimately, we are contributing toward the set of tools that clinicians will have that will enable them to map the brain with even greater confidence and precision, and personalised to each patient,” said Mahon. “The big goal is to translate scientific insights into solutions that improve people’s lives. We will meet that goal by building tools that enable the best possible outcomes in neurosurgery patients, both in terms of neurocognitive function and quality of life, and ultimately, in terms of survival.”
Source: Carnegie Mellon University

