About 1% of Hospitalised COVID Patients Develop Neurological Complications
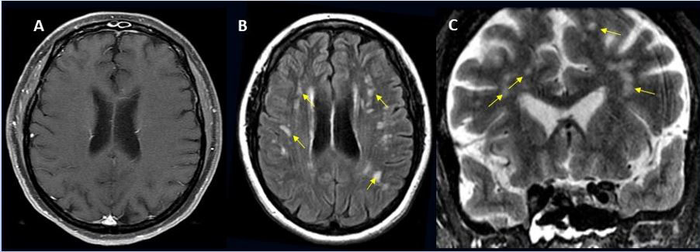
Approximately one in 100 patients hospitalised with COVID will likely develop complications of the central nervous system, according to a large international study. These can include stroke, haemorrhage, and other potentially fatal complications. The study was presented at the annual meeting of the Radiological Society of North America (RSNA).
“Much has been written about the overall pulmonary problems related to COVID, but we do not often talk about the other organs that can be affected,” said study lead author Scott H. Faro, MD, FASFNR, professor of radiology and neurology at Thomas Jefferson University. “Our study shows that central nervous system complications represent a significant cause of morbidity and mortality in this devastating pandemic.”
Dr Faro initiated the study after finding that only a small number of cases informed existing literature on central nervous system complications in hospitalised COVID patients.
To build a more complete picture, he and his colleagues analysed nearly 40 000 cases of hospitalised COVID patients, admitted between September 2019 and June 2020. Their average age was 66 years old, and two thirds were men.
Confusion and altered mental status were the most common causes of admission followed by fever. Comorbidities such as hypertension, cardiac disease and diabetes were common.
There were 442 acute neuroimaging findings most likely associated with the viral infection, with central nervous system complications in 1.2% of this large patient group.
“Of all the inpatients who had imaging such as MRI or a CT scan of the brain, the exam was positive approximately 10% of the time,” Dr Faro said. “The incidence of 1.2% means that a little more than one in 100 patients admitted to the hospital with COVID are going to have a brain problem of some sort.”
Ischaemic stroke, with an incidence of 6.2%, was the most common complication, followed by intracranial haemorrhage (3.72%) and encephalitis (0.47%).
A small percentage of unusual findings was uncovered, such as acute disseminating encephalomyelitis, an inflammation of the brain and spinal cord, and posterior reversible encephalopathy syndrome, a syndrome that mimics many of the symptoms of a stroke.
“It is important to know an accurate incidence of all the major central nervous system complications,” Dr Faro said. “There should probably be a low threshold to order brain imaging for patients with COVID.”
Source: EurekAlert!


