A Look Back at 2021

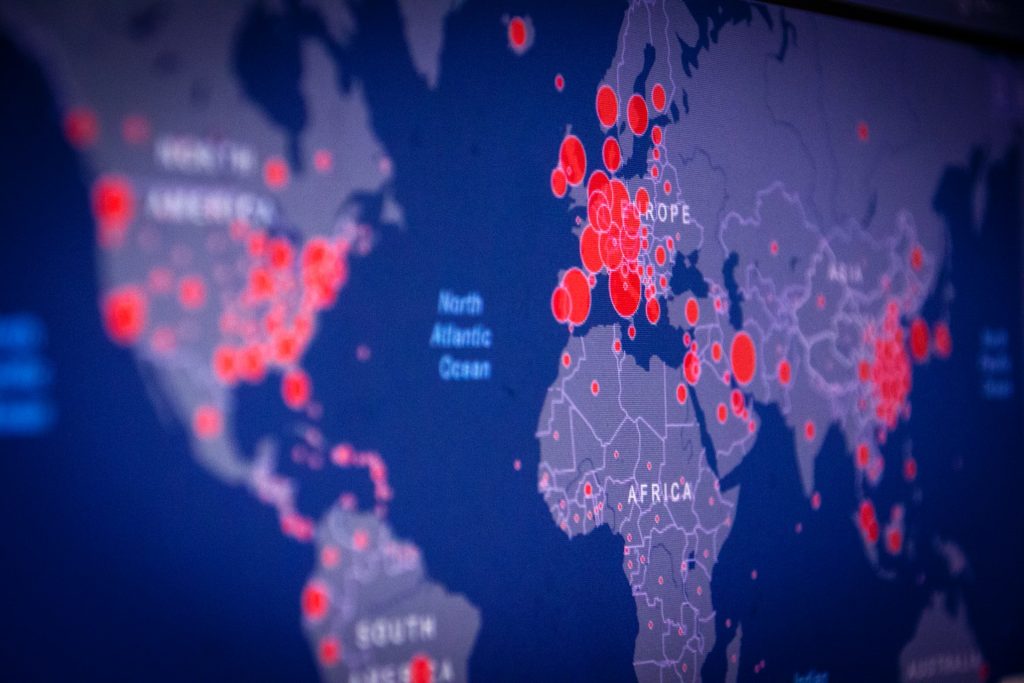
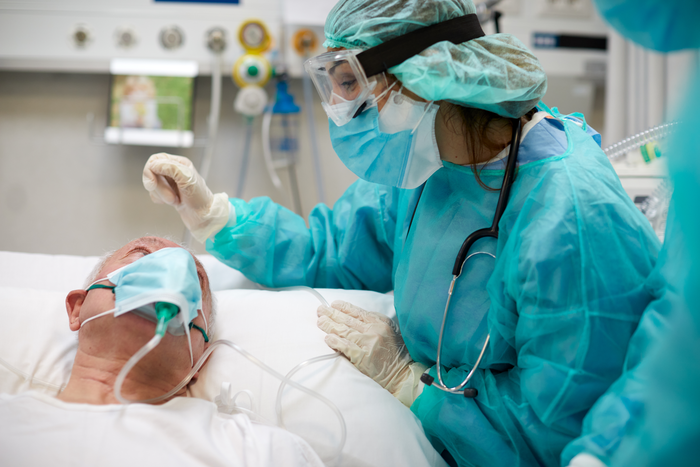
The start of 2021 saw South African hospitals battling for resources amid a COVID surge, and planning for what would be a very controversial and drawn-out vaccination programme which would be partly paid for by the overflowing coffers of the country’s medical aid schemes. Indeed, there was a real concern that the as-yet-to-be-named Beta variant would evade vaccines, which would prove to be true – and a story which would be repeated with the Omicron variant later in the year. In China, the start of an investigation into the origins of the SARS-CoV-2 virus in Wuhan was stymied by the Chinese government denying them entry.
The middle of the year saw the Third Wave, now driven by the highly transmissible Delta variant which had ravaged India earlier in the year. Production setbacks further dogged South Africa’s vaccine programme as millions of Johnson & Johnson vaccines were deemed unfit for use. In Brazil, deaths passed half a million amid condemnation of the mishandling of the COVID pandemic by its President Jair Bolsonaro. Economic frustration, stoked by political manoeuvring around the trial of former President Jacob Zuma, saw much of the country erupt in looting and violence. This would seriously damage COVID vaccination and surveillance efforts in the affected areas, particularly KwaZulu-Natal.
Statins seemed to be losing some of their bad image as new studies revealed that they were not associated with cognitive decline, following on from a 2020 study showing many of their feared side effects were the result of the ‘nocebo’ effect. The US government initiated a probe into how a controversial drug for the treatment of Alzheimer’s disease managed to receive approval despite no evidence of benefit. Dr Zweli Mkhize stepped down as Health Minister amidst revelations about procurement irregularities relating to the Digital Vibes contract.
Towards the end of the year, South African vaccination rates fell due to a combination of factors: vaccine hesitancy, apathy and difficulty servicing remote areas. Omicron was detected in late November, immediately raising alarm due to the extremely large number of mutations it possesses. In response, countries around the world announced immediate travel bans or heightened quarantine restrictions. However, these proved futile as the highly contagious Omicron was already loose in the borders of many countries, rendering the controversial containment efforts moot.
Fortunately, early signs from Netcare showed that Omicron caused less severe disease. By year end, new effective COVID treatments were going through these stages of their final approval. Merck’s Molnupiravir (Lagevrio) had shown promise for the treatment of COVID, though later analysis with additional data showed it to be less effective than believed. Expected production for Pfizer’s nirmatrelvir (Paxlovid) was expected to increase to 80 million courses after results showed an 89% reduction of hospitalisation or death for outpatients. As the year closed, there was some good news for South Africa’s economy as travel bans were lifted – though the countries imposing them now had Omicron surges of their own to contend with.